
This exhaustive report illuminates the inner workings of the Michigan Education Association's health insurance division, known as MESSA. It documents how tens of millions of the public's education tax dollars are wasted each year on uncompetitive teacher health insurance, and how MESSA is part of a systematic plan to subsidize the MEA's basic operation and political activity. 64 pages.
Over one year ago, the Mackinac Center for Public Policy was approached by a concerned parent who had watched his school district, during a heated contract negotiation, spend over half a million dollars more for teacher health insurance than seemed reasonable. In addition to the excessive costs, the fact that the insurance provider was a subsidiary of the Michigan Education Association (MEA) caught his attention. The Mackinac Center investigated and, after nine months of research, has summarized its findings in a report titled Michigan Education Special Services Association: The MEA's Money Machine.
This report documents two important findings: (1) tens of millions of education dollars are wasted each year on unusually costly teacher health insurance; and (2) the MEA's insurance subsidiary is part of a systematic plan to use money intended for education to subsidize the MEA's basic operations and political activity.
The Michigan Education Special Services Association (MESSA, pronounced MAY-sah) is a wholly-owned, non-profit subsidiary of the MEA. It is a third party administrator of health insurance benefits to public school employees who are MEA members. MESSA contracts with the school district to provide benefits, and then administers insurance actually underwritten by Blue Cross/Blue Shield of Michigan. MESSA keeps a portion of the school district's payment to cover its "administrative" costs.
MESSA currently dominates the public school employee benefit market, providing insurance to over 300 of Michigan's 524 K-12 school districts. MESSA took in over $360 million in premiums in 1992 alone. To put this amount in perspective, it is roughly 6 percent of the total revenue cut under Senate Bill 1, which eliminated the local school operating property tax.
The following describe the reports two major findings:
1. Excessive Costs for Insurance Benefits
There are two reasons why the cost of MESSA health insurance is excessive.
One is the extremely high administrative costs of the MESSA/Blue Cross operating
agreement. In addition to high salary and benefit levels for MESSA employees and questions of productivity, both MESSA and Blue Cross have separate claims processing facilities that require redundant expense. MESSA also supports the extensive data processing facility that the MEA uses for its basic operations and political activity. MESSA and the MEA also "share" employees for lobbying and other purposes.
School districts also have a difficult time soliciting competitive bids because MESSA, unlike other insurance providers, refuses to provide a claims history. A claims history is a record of the bills submitted by the school district employees for payment or reimbursement. These are used as a basis for bids by competitors.
The second reason why the cost of MESSA insurance is excessive is the design of the benefit packages. MESSA benefits are extremely generous, and cover most health-related procedures in full or nearly full. These benefits are well in excess of what comparable private employers in the same area provide their employees. One reason for this is that the MEA likes to compare benefits to other school districts around the state, which already may be at high levels, rather than other local employers.
2. How MESSA Supports MEA operations and political activity.
During the mid-1950's to early 1960's, the MEA provided benefits as a way to entice school employees to join it rather that its rival, the Michigan Federation of Teachers. MESSA was created in 1960 as part of an orchestrated effort to use insurance benefits to gain union support and as a source of revenue to fund union operations.
Today, MESSA pays the MEA millions of dollars in exchange for having local MEA bargaining agents pressure school districts into purchasing expensive MESSA insurance. The benefits serve to keep many union members supportive of the union even though they may disagree with the MEA's position on political or educational issues.
Both the MEA and MESSA fund lobbying staffs in Lansing, and the MEA is the state's largest single supporter of political candidates through its political action committee. The influence of the MEA is one of the main reasons Michigan school reform efforts have been thwarted at nearly every turn.
The study recommends several ways to minimize the harm the current MEA/MESSA relationship is imposing on school districts. First, the Public Employment Relations Act, which mandates collective bargaining with public school employees, should be amended to either exempt teachers altogether or eliminate health insurance and other benefits as a mandatory topic of bargaining. The former would still allow teachers to join a union, but not be forced into membership or support. The latter would still require school districts to bargain wages and other conditions of employment, but they would have more freedom to select insurance providers based on cost and merit, not political pressure.
In the mid-1950's and early 1960's, as the Michigan Education Association (MEA) was making its transition from a professional teacher's association to a militant labor union, the organization's leaders hit upon a brilliant plan to shore up support for their growing organization. The plan was so ingenious, in fact, that it is responsible in part for catapulting the MEA to its current position as one of Michigan's most powerful political forces and the most influential state affiliate of the National Education Association. It is also a plan that is being examined, and in some cases duplicated, by labor organizations across the country.
The plan was simple in concept. Since 1939 the MEA had worked with an agent of the Hoosier Casualty Company of Indianapolis, Indiana to provide its members with limited insurance coverage, usually paid by the MEA member. Facing competition from the Michigan Federation of Teachers, the MEA's rival union, the MEA began to augment existing insurance benefits as a way to entice teachers to support their organization. The union leaders recognized that they would have maximum control over the insurance program if the union itself were in charge of the insurance plan. Since Michigan law prevented the MEA from acting as an agent, it created in 1960 a wholly-owned non-profit subsidiary, the Michigan Education Special Services Association (MESSA). MESSA acted originally as a third party administrator, handling the policies and claims which were paid by a separate insurance underwriter.
The genius of the arrangement after 1960 was that MESSA would pay the MEA to bargain MESSA benefits during contract negotiations, thereby becoming a source of revenue to subsidize the union's rapidly expanding field operations staff. While in the beginning MEA members paid the premiums, school districts were increasingly pressured during negotiations to make payments directly to MESSA as part of the union contract. Thus the machinery was in place to develop what is today a complex arrangement of subsidiaries and fund transfers that provides revenue and services to support the MEA and its political operations, while wasting millions of dollars intended for education. MESSA is, in effect, an insurance company that uses mandatory collective bargaining laws to sit across the negotiating table and pressure school districts to purchase its coverage.
Today, in more than 300 of Michigan's 524 public school districts, the rising cost of education is linked to this arrangement, which often goes unnoticed by many school boards, as well as the parents and taxpayers who ultimately fund the districts. While there is no question that public school employees deserve decent, well-administered insurance benefits, the benefits packages now negotiated by these school districts from MESSA offer unreasonable coverages and unusual provisions that simply cannot be justified on their merits. Those school boards that do recognize the pitfalls of MESSA insurance are often placed in the no-win situation of either agreeing to fund MESSA coverage or face a disruptive and illegal teacher strike that would cheat children of their education.
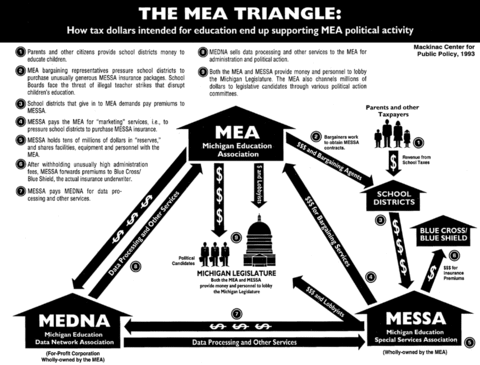
This report documents the relationship between the MEA and its MESSA subsidiary, as well as the other MEA subsidiaries that affect it. Figure 1 illustrates the basic elements of this relationship. For those who are concerned about the quality of education in Michigan, an understanding of this relationship explains much about why Michigan citizens are not getting full benefit from the money that is dedicated to education, as well as why education reform has been thwarted at nearly every turn. But in order to understand MESSA's success and the power it provides, it is important to understand something about the MEA.
The most formidable union in the state of Michigan has nothing to do with auto workers, teamsters, service employees, or food workers. Although it is merely a state affiliate of a national organization, it happens to be the most powerful of the state affiliates, having provided the national union with its current two top executive officers. It has the ability to coordinate shutdowns of school districts, as it did to the Kalkaska schools in March of 1993.1 It can force membership on anyone who is eligible through the "agency shop" and collective bargaining laws which it helped establish. Its members often disregard the law, by striking in plain violation of Michigan's Public Employment Relations Act.2 It need not fear retribution from Michigan's lawmakers, since it manipulates the political process through campaign contributions. In fact, it has one of the wealthiest political action communities in the state, sharing millions of dollars with its political allies. (See Appendix I for a list of legislators who receive MEA support). In 1988, for example, it was the largest single contributor to a petition drive in support of Medicaid-funded abortions. In 1989, it spent $1.5 million to promote an increase in the state sales tax. Many of its members participate on decision-making bodies throughout Michigan, such as Barbara Roberts Mason, who is on the State Board of Education. It organizes boycotts of major Michigan corporations, as it did it 1981, when it began a boycott of the Amway Corporation.
Michigan's most formidable union is the labor representative of some 120,000 public school employees-the Michigan Education Association. A state affiliate of the National Education Association, the MEA is the larger of Michigan's two statewide teachers’ unions. Ever since the widespread unionization of public employees in the early 1960s, the teachers' unions have gained considerable control over public school teachers in the state of Michigan by compelling them to join their ranks. And the cost has not been cheap. School district funds are continually diverted from classrooms in order to pay for contract negotiations, strike costs, lawyer fees, litigation expenses from labor disputes, and other union-prompted expenditures. Although it contends otherwise, the MEA often puts the concerns of its members before the concerns of students, as demonstrated by outbreaks of illegal teacher strikes, school district closings, increasing salaries often at the expense of other programs, and a lobbying division with only a secondary concern for education quality.
As mentioned previously, the strength of the MEA dates back to the 1960s, when the MEA leadership discovered a new agenda and new ways of acquiring influence. Keith Geiger, Terry Herndon, and Don Cameron were the three labor activists who turned the MEA from a professional association into a militant labor union, and eventually did the same thing for the NEA.
The MEA is distinguished from other teachers' unions in the sense that it not only represents the interests of teachers in contract negotiations, it also operates a multimillion dollar conglomerate out of three interconnected office buildings in East Lansing. The three subsidiary operations of the MEA provide millions of dollars in revenue to the union, with activities ranging from administration of insurance benefits to data processing.3 In addition, the property holdings and capital of the subsidiaries provide the MEA with even greater equity and resources. But aside from tangible benefits, the subsidiaries also give the MEA a powerful way to manipulate its membership and spread its range of influence throughout the state.
The three subsidiary corporations which are owned and controlled by the Michigan Education Association are the Michigan Education Special Services Association, Michigan Education Association Financial Services, and the Michigan Hucation Data Network Association .4
The Michigan Education Special Services Association ("MESSA," pronounced
MAY-sah) was incorporated by the MEA in 1960 as a wholly-owned, not-for-profit subsidiary.
MESSA administers insurance benefit programs to participating MEA members, including life,
accidental death and dismemberment, disability, health, dental, and vision coverage. Local
affiliate unions of the MEA can bargain MESSA insurance plans into their labor contracts
with their respective school districts. In such cases, the corporation which administers
insurance benefits to the school district's employees is also a part of the organization
which represents the school district's employees during contract negotiations. This gives
the MEA unprecedented leverage in controlling the compensatory benefits received by its
members.
In 1973, the Internal Revenue Service informed the MEA that MESSA's not-for-profit
status could be revoked unless MESSA stopped offering group automobile insurance and
variable annuity programs to MEA members. In response to this threat, the MEA created the
Michigan Education Financial Services Association, which is now known as MEA Financial
Services. This subsidiary provides MEA members with numerous investment services,
including annuities, investment retirement accounts, credit cards, mutual funds, auto
owners insurance, and home owners insurance. With MEA Financial Services, the MEA is able
to financially assist its members beyond the scope of guaranteed insurance
coverage by acting as an "investment counselor" of sorts.
The Michigan Education Data Network Association ("MEDNA," pronounced MED-nah) was chartered in 1982 as a wholly-owned for-profit subsidiary of the MEA. Unlike the other subsidiaries, MEDNA's purpose is to service the MEA rather than the MEA's members. MEDNA provides a wide range of clerical and administrative services to the MEA and its other subsidiaries, including data processing, communications, and accounting. In exchange for these services, MEDNA receives compensation from the MEA and its other subsidiaries. As will be discussed later, MEDNA is a resource pool for the whole MEA conglomerate.
This report is concerned with the MEA subsidiary of most interest and greatest importance to the parents and taxpayers of Michigan-the Michigan Education Special Services Association. MESSA is important for several reasons. In the past decade, MESSA has attempted to become a monopoly in the market for administration of insurance benefits to public school employees, and it has done so by maneuvering its way into labor contracts with the MEA's assistance. In order for MESSA to administer insurance to a school district's employees, a MESSA insurance plan must be negotiated with the school district during the collective bargaining process. Since the MEA is the collective bargaining representative of most public school employees and the parent corporation of MESSA, MESSA gets a disproportionate share of the market. This holds special significance for the school districts that suffer the financial consequences of reduced competition in the market for insurance coverage of their employees.
With $360 million in 1992 premiums alone, MESSA currently receives public funds from approximately 60 percent of Michigan's school districts in exchange for insurance coverage of school district employees, including teachers, support staff, and administrators.5 The majority of these revenues (92.5 percent in 1992) are used to pay for the cost of insurance benefits. Evidence suggests, however, that MESSA's benefit costs are abnormally high, due to a number of factors which relate back to excesses in the design of the overall benefit packages. In addition, MESSA's revenues which do not apply to benefit costs are used for purposes which are also cause for concern. Almost all of MESSA's remaining revenues are either allocated to unusually high operating expenses or deposited in huge cash reserves. As it turns out, almost one-third of MESSA's operating expenses are for "services" rendered by other corporations in the MEA conglomerate.
An examination of MESSA is particularly relevant with the recent approval of Senate Bill 1, which eliminated $6 billion in property tax-based school operating funds. Consider that MESSA's premiums are the equivalent of over 6 percent of the eliminated taxes. Given the facts that MESSA has established a formidable base of political power through the lobbying activities of the MEA, MESSA receives hundreds of millions of tax dollars every year through its benefit contracts with school districts, and school districts more often than not yield to MESSA coverage when it is demanded by the teachers' union, MESSA plays an important role in determining tax policy for the state of Michigan.
For over 30 years, MESSA has administered innovative but costly insurance benefits to public school employees throughout Michigan at the expense of school districts, and, ultimately, the taxpaying public. Even though MESSA is a major recipient of funds intended to finance public education, the public remains mostly uninformed about this operation. This report provides specific information about MESSA, elaborates on the various causes for concern about MESSA, and answers the fundamental question: Does MESSA, as a recipient of public funds, operate in the public's best interest?
The Michigan Education Special Services Association was created by the Michigan Education Association in 1960 for the purpose of administering insurance benefits to members of the teachers' union. MESSA now manages contracts for insurance benefit provision in approximately 60 percent of Michigan's 523 K-12 public school districts.6 By having its own insurance administrator, the MEA is able to control the amount and quality of benefits received by its members. The programs administered by MESSA include life, accidental death and dismemberment, disability, health, dental, and vision coverages. However, MESSA is most often associated with its six health insurance plans-Super Med I, Super Care I, Super Med II, Super Care II, MESSA 250/20, and MESSA Limited. Of these plans, the Super Med and Super Care plans provide the better benefits and are purchased with greater frequency. This report is predominantly concerned with MESSA's health insurance plans, because they constitute the largest portion of MESSA's business.
Although MESSA is an administrator of insurance benefits, it does not meet the general criteria of an insurance company. This distinction can often lead to misunderstandings about what MESSA does, but in order to qualify as an insurance company, MESSA would have to assume risk for losses and gains on its insurance plans. MESSA only administers insurance benefits which have been underwritten by other companies, so it is considered to be a third party administrator (TPA) of insurance. (It must be noted, however, that the nature of the operating relationship with Blue Cross/Blue Shield of Michigan has raised questions as to whether MESSA does actually assume risk, and should be subject to the general provisions of the insurance code.) TPAs are quite common in the insurance industry; the Society of Professional Benefit Administrators reports that TPAs currently administer insurance plans to just under half of all U.S. workers.7 As a TPA, MESSA develops and holds various group insurance policies that are underwritten by a licensed insurer pursuant to a contract. The policies are dispensed to MESSA's participants through MESSA itself, rather than through the underwriters. In short, MESSA is an administrator of insurance benefits that sells insurance plans, but does not underwrite the plans.
The classification of MESSA as a TPA is mainly for the regulatory purposes of the Michigan Insurance Code. For tax purposes, MESSA is classified as a not-for-profit, tax-exempt voluntary employee beneficiary association (VEBA).8 To qualify as a VEBA, MESSA must guarantee that its members have an employment related bond-public education-and it must maintain "an arm's length relationship" in financial dealings with affiliated corporations, such as the MEA.9
MESSA operates in the narrowly defined market for administration of insurance to public school employees. The market itself is not very competitive, given MESSA's commanding position relative to other firms. Technically, MESSA competes with other third party administrators, insurance companies, and health care corporations that also deal in the business of administering insurance benefits to public employees. For example, the School Employees Trust, Inc. ("SET"), a division of the Michigan Association of School Boards, is a third party administrator that has competed with MESSA for the past twenty years (even though both MESSA and SET were founded by the same person).
No other state affiliate of the National Education Association has been able to duplicate the MESSA concept. Some attempts have been made, yet none have succeeded. There is speculation that MESSA is a precedent for the NEA itself, now that the NEA's life insurance operation resembles the MESSA concept. Government records indicate that the NEA's comparable not-for-profit subsidiary involved in membership services has encountered similar success: the NEA Members Insurance Trust has accumulated net assets exceeding $65 million.10 Nevertheless, the MEA has created an elaborate scheme that is the envy of NEA affiliates around the nation.
In almost every case, MESSA insurance benefits are provided to public school employees because the teachers' union and the local school district have agreed to a MESSA insurance plan in their labor contract. In some instances, the school district will also purchase MESSA coverage for administrators and other non-unionized employees. Once the district and the union have agreed to a specific MESSA insurance plan, the school district enters into a contract with MESSA and becomes a "customer" of MESSA. The role assumed by MESSA is that of the middleman: Rather than have insurance benefits administered directly by an underwriter, the school district purchases its insurance through a third party. This practice is quite common among school districts.
Anyone who is covered by a MESSA plan is called a "member" of MESSA. Membership is restricted to past and present employees in public education, including teachers, administrators, and support personnel. Specifically, the MESSA membership criteria state that eligible participants must have some relation to the teachers' union, either as members of the MEA, employees of the MEA and its subsidiary corporations, employees of school districts where the MEA has bargained MESSA benefits for its members, and qualified retirees of the public education sector.
In effect, MESSA operates as an insurance agency servicing public school employees throughout the state of Michigan, with representation of commercial carriers including the Equitable Life Assurance Society, Delta Dental, Blue Cross/Blue Shield of Michigan, and Lincoln National Life. In fact, the Michigan Insurance Bureau reports that MESSA is licensed to perform the activities of an insurance agent.
Premiums for MESSA insurance are collected by MESSA from customer school districts on a monthly basis. A handful of members also purchase insurance from MESSA on their own without the intervention of a school district. The premiums for MESSA coverage are based upon actuarial calculations of the financial risk assumed by the underwriter and MESSA's anticipated costs of administration. According to MESSA, it now covers some 80,000 public school employees and 200,000 of their dependents with annual premiums of approximately $360 million.
In its capacity as a third party administrator, MESSA is first responsible for designing the various benefit structures of its insurance plans. Once a plan has been created, MESSA locates an underwriter for the plan and enters into an operating agreement which identifies the terms for compensation and the division of administrative responsibilities. After receiving monthly contributions from its customers, MESSA pays a separate premium to the plan's underwriter as the purchase price of actual coverage against losses for its members. MESSA also deducts certain allowances from its total revenue collections for the costs of administering benefits.11 Among its principal administrative duties, MESSA performs eligibility determinations, enrolls and counsels participants, handles certain claims for losses, establishes the claims appeal procedure, and collects premiums. However, MESSA is not the exclusive administrator of its insurance plans. In the case of its health plans, for example, MESSA and Blue Cross/Blue Shield of Michigan co-administer the programs, with MESSA and Blue Cross both processing specific claims.
When MESSA first began operating, it was little more than a fledgling insurance agency. As MESSA's market share expanded, so did the size of its operations. The current organization of MESSA is so expansive that it now requires a 70,000 square foot office building, a staff of approximately 200, and a specific delegation of responsibilities through three departments.
Warren Culver, a former employee of both the MEA and MEDNA, has been the executive director of MESSA since 1990. He serves as the chief administrative officer, with ultimate responsibility for administration, sales, performance, development, relations with the MEA and its other subsidiaries, and the regular daily operations of MESSA. Currently, there are three departmental directors who report directly to the executive director and hundreds of others who report indirectly to him.12 The three departments of MESSA include Marketing and Field Services, Benefits Administration, and Healthcare Resources.
The Department of Marketing and Field Services consists of approximately 30 staff members, including the MESSA field representatives who act as liaisons between MESSA and its membership. Under the leadership of Jim Hobson, this department performs certain membership services, such as answering members' questions, handling account renewals, and quoting prices for customer school districts. Field representatives, who usually have background experience as licensed insurance agents, are assigned to specific regions of the state where they intervene between MESSA and its individual members over concerns related to administration of insurance benefits. MESSA's division of field representatives is separate from the MEA's Uniserv division of professional contract negotiators, although they apparently share many of the same duties, such as counseling MEA members about MESSA's programs.
At the core of MESSA's operation is its largest single department, Benefits Administration. With a staff of around 140, the Department of Benefits Administration handles all claims from members, as arranged for in MESSA's operating agreements with its underwriters. In addition to processing claims and coordinating benefits, this department administers certain MESSA programs, such as claims evaluation and case management. This aspect of MESSA's operations is directed by Ann Purvis.
Under the directorship of Chuck McMillan, the Department of Healthcare Resources is primarily focused on MESSA's health insurance programs, which cover the vast majority of MESSA participants. The activities of this department are based upon MESSA's contract for underwriting services from Blue Cross/Blue Shield of Michigan. With a staff of around 25, this department helps coordinate the options given to MESSA members for receiving medical services, in conjunction with Blue Cross.
Almost all of MESSA's clerical work is handled by the Michigan Education Data Network Association, which is, in effect, an indirect department of MESSA. Among other things, MEDNA provides MESSA with financial services, personnel services, property maintenance, and computer operations/maintenance. In fact, Dick Ringstrom, MEDNA's director of data processing, is a former director of marketing and field services at MESSA. Of greatest importance to MESSA is MEDNA's responsibility for operating the central processing unit of MESSA's complex computer network.
Regulatory Considerations. Several government offices monitor the activities of MESSA, mostly within the Michigan Departments of Commerce and Labor. Since MESSA's primary business function is third party administration of insurance, it must report to the Insurance Bureau of the Michigan Department of Commerce. The Insurance Bureau licenses MESSA and its managers, ensures compliance with the law, examines the financial solvency of the corporation, certifies MESSA insurance plans, and handles all complaints against MESSA. In addition, MESSA is subject to the regulations of the insurance industry contained within the Michigan Insurance Code. In the past, MESSA's attorneys have contended that MESSA's business activities do not constitute transactions of insurance for the regulatory purposes of the Code.13 Rather, they have contended that MESSA is regulated by the Third Party Administrator Act of 1984, which provides the specifications and guidelines for administering insurance plans which have been underwritten by a separate commercial carrier. Yet according to Jean Carlson, director of the Insurance Bureau's Office of Policy, MESSA must comply with the Insurance Code, because it functions as an insurance agent and because the Third Party Administrator Act is a "supplement" to the Code.
Judicial Considerations. Several court cases involving the MEA have secured MESSA's hegemony in the market for administration of insurance benefits to public school employees. The two most important cases were both decided by the Michigan Court of Appeals during the 1980s. In the 1981 case of Houghton Lake Education Association v. Houghton Lake Board of Education, the Court ruled that a school district cannot unilaterally choose the most cost-effective insurance administrator once the contents of an insurance plan have been negotiated.14 The Court stated that the choice of an administrator for the plan is not a managerial decision reserved by the school district, but a bargaining issue which must be resolved through negotiations with the labor union and identified in the labor contract. In its 1986 decision in MEA/NEA v. St. Charles Community Schools, the Court ruled that insurance benefits are a mandatory topic of all contract negotiations involving school districts and the teachers' union.15 The bargainers do not have to settle on the issue, but a discussion of insurance benefits must be incorporated into the overall collective bargaining process if a negotiating party raises the issue. As a result of both cases, school districts have been put at a disadvantage, because they can neither avoid the issue of insurance nor decide who the plan administrator will be without the consent of MESSA's parent corporation-the MEA. Not all MEA local affiliates bargain for MESSA coverage with the same intensity and not all school districts bow to the union's pressure, so some school districts have avoided MESSA, despite the fact that two court decisions now stand which have cleared the way for MESSA to dominate its market.
As of late, no final court decision has adversely impacted MESSA's ability to conduct business; however, a case is now pending before the Michigan Court of Appeals which could prevent MESSA from making unilateral changes in its insurance plans during the course of a contract period.16 This particular case, IEA/MEA and MESSA v. St. Clair Intermediate School District, is discussed later in this report.
The importance of MESSA to the MEA extends far beyond the unique insurance benefits provided t I o MEA members by MESSA. More importantly, MESSA is an effective program for controlling the loyalty and support of the union's members, thereby giving the MEA the membership strength and financial resources required to successfully advance its agenda throughout the State of Michigan. That agenda contains several controversial goals for labor, education, and other political issues.17
The program is so effective, in fact, that a recent survey of MEA members revealed that they value MESSA health benefit packages over all other services administered by the MEA.18 Considering that MESSA's health plans cover almost any medical expense in full or close to full, this comes as no surprise.19 MESSA benefits are also tax-exempt because they are part of an employee compensation package. Moreover, everyone who is enrolled in a MESSA plan can rest assured that their insurance administrator is on their side; MESSA admits that it is biased toward school employees from the outset. In the 1981 Houghton Lake case, for example, MESSA testified that it will interpret benefit contracts in favor of public school employees, even if the result is higher costs to school districts.20
The MEA tells its members that without MESSA, they could not obtain comparable health insurance unless they were willing to give up liberal benefits and user-friendly service. For example, a promotional flyer distributed by the MEA informs MEA members that:21
"Equivalent coverage plans can't provide [MESSA advantages], so these plans can't be equivalent!"
"You do not have to deal with insurance carriers who don't understand your unique needs as an MEA member."
"MESSA was designed to service MEA members."
"Your health insurance is an important part of your compensation package. It should not be under the control of anyone but you and your organization: the MEA."
MEA members realize the value of MESSA, and they will defend a generous benefit. Members also realize that without the MEA, they could not have access to MESSA, so they will defend the MEA. In this sense, MESSA fosters support for the teachers' union.
The MEA's chief lobbyist, Al Short, conceded the point when he recently stated: "You take members that don't believe in collective bargaining, that don't believe in our political ends, but you talk to them about MESSA, they'll stand in the middle of a highway to defend it. That's the tie."22 In light of MESSA, many MEA members seem to forget their differences with the union. Once the MEA has the cooperation of its members, it can go ahead with its agenda and support political causes that many of its members find offensive. Other results from the afore mentioned survey of MEA members exemplify the discontent:
86 percent of leaders in the union are bothered that "the MEA takes stands I do not agree with."
69 percent of teachers are bothered that "the MEA takes stands I do not agree with."
55 percent of teachers are bothered that "the MEA is too liberal."
64 percent of teachers are bothered that "the MEA is mainly committed to union goals, not professional goals for education."
75 percent of teachers are bothered that "the MEA gets involved in issues, like abortion, that have nothing to do with education."
Not only does the MEA acquire the support of its membership through MESSA's programs, it can also induce significant financial support from its membership through MESSA. As long as the MEA can guarantee that its members are loyal to the union, it can also guarantee that members will pay their dues without objection or reservation. Since dues are the MEA's primary source of income, providing the union with around $30 million in 1992, it is crucial that the MEA ensure its financial viability through effective programs such as MESSA.23
Across the state of Michigan, public school districts are suffering at the hands of the Michigan Education Special Services Association. In the market for administration of insurance benefits to public school employees, MESSA has acquired numerous unfair advantages which have essentially restrained its competition and prevented school districts from locating an objective, cost-effective administrator of insurance. Ever since the Michigan Education Association established its lucrative insurance enterprise, most school districts no longer select their insurance administrator based on its quality and efficiency, but rather for its connection with the teachers' union. Consequently, MESSA now administers insurance to nearly 60 percent of all Michigan school districts, even though its benefit packages are designed with several apparent deficiencies (discussed in subsequent sections of this report).
In short, MESSA's unfair market advantage is that it has a privileged alliance with the MEA. No other insurance administrator in the state enjoys the benefit of having its programs sponsored by the bargaining representative of over 120,000 public school employees. The representation provided to MESSA by the MEA amounts to an unfair advantage for MESSA because the MEA can mobilize its interests in order to advance or protect the interests of MESSA. Hence, not only must school districts contend with the MEA during salary negotiations, they must also accommodate both the MEA and its insurance subsidiary on the issue of employee insurance benefits. The total effect of this biased treatment is that competition has been stifled in the market for administration of insurance benefits to public school employees, producing a hostile market environment for school districts to shop in.
The initial reason why MESSA has cornered the market for administration of insurance benefits to public school employees is because the state of Michigan has fundamentally outlawed competitive bidding of insurance plans in school districts. The 1981 court ruling in the case of Houghton Lake Education Association v. Houghton Lake Board of Education determined that school districts have a duty to negotiate with the teachers' union over the amount of insurance benefits given to school employees along with the specific company which will administer the benefits.24 Ever since the ruling was handed down, the impact on public education has been detrimental, because it cleared the way for an insurance administrator supported by a teachers' union to dominate the market without regard to cost.
The process of negotiating insurance benefits usually begins with the school district and the teachers' union individually choosing the amount of benefits and an administrator of those benefits. These decisions become the focal point of their discussions. Due to the fact that a school district cannot contract with a quality, cost-effective insurance administrator on its own, firms must compete with one another for the favor of both the district and the teachers' union. School districts tend to favor those firms which can deliver the agreed upon benefits at the lowest possible cost, but since MESSA is a subsidiary of the MEA, the teachers' union will always favor its own administrator of insurance benefits. The union typically has little concern about costs, because the school district picks up the tab for insurance benefits.
When the time comes for the union and the district to negotiate the administrator of insurance benefits, the MEA consistently pushes for MESSA. The MEA even requires that its bargaining agents attempt to obtain MESSA coverage for a school district's employees whenever contracts come up for renewal. Consequently, school districts are unable to bargain on a level playing field with the union over insurance benefits. 'Me teachers' union can simply bargain MESSA coverage into a labor contract under the threat of strikes or prolonged negotiations.
School boards throughout the state recognize that any threat to MESSA is grounds for a strike by the MEA. Unfortunately, the state of Michigan generally does not enforce its own laws as they pertain to strikes by public school employees. The Public Employment Relations Act which governs the conduct of the MEA explicitly makes it illegal for public school employees to strike. Yet, teachers strike with regularity and are rarely penalized for their actions. In this sense, the strike option gives authority to the MEA for imposing MESSA insurance plans against the will of school districts. After all, school districts rarely have the power to combat a force of striking employees. This gives MESSA a considerable advantage in the bargaining process, which prevents many school districts from seeking more affordable insurance administrators. In fact, the few eligible school districts which do not have MESSA coverage are those that have the unusual strength and resources to resist the MEA.
The loss for school districts is that they cannot control the costs of employee insurance, because they must decide their insurance administrator in conjunction with an organization that cares more about benefits than costs and has the bargaining leverage to impose its will over school districts. For example, in addition to demanding MESSA insurance plans, the MEA also insists that school districts not minimize their cost liabilities by setting a limit on annual premium payments.25 This gives MESSA the flexibility to increase premiums with the guarantee that school districts will have to make payment. Since other insurance administrators cannot contract with the dominant bargaining agent as can MESSA, any competition to MESSA is nudged out of the market, which also hurts school districts by forcing them to patronize an administrator that has no incentive to price competitively.
The superintendent of the Hemlock School District demonstrated the typical concern among school administrators about the absence of competitive bidding and the presence of MESSA:
Rising health costs represent the most inflationary and uncontrollable line item in all school budgets. One of the main problems is that school districts have bargained certain carriers into their master contracts, which eliminates the competitive bidding process. We believe legislation should be enacted that would supersede any such contractual language and require school districts to put their insurance out for bid on a required cycle and award to the lowest qualified bidder. This is an oversimplification of a somewhat complex and highly political problem in that MESSA (MEA) is the major health-care insurance provider in our schools. 26
As long as the MEA can bargain for its own insurance provider, school districts will continue to suffer and MESSA's competitors will not have a realistic chance of actually vying for school district business.
Many school districts have also complained about MESSA's infiltration into the collective bargaining process. They contend that MESSA advises the bargaining representatives of the MEA in the same way a trainer coaches the fighter as he spars with his competitor. This third party intrusion into the bargaining process, they contend, is a violation of their right to exclusive negotiations between employees and their employer. Surely, the union would object if school districts involved a council of advisory taxpayers in labor negotiations. Towards the end of the last decade, 15 Michigan school districts filed a complaint when the presence of MESSA in collective bargaining talks began to infringe upon their rights as parties to an agreement. The case was litigated before the Michigan Court of Appeals, where an earlier dismissal was upheld.27
The complaint of the school districts was based upon concerted actions taken by MESSA with the MEA's apparent counsel. In 1985, MESSA changed the underwriter of its health insurance plans from the Equitable Life Assurance Society to Blue Cross/Blue Shield of Michigan. The change in underwriters presented a dilemma to MESSA, because all of its pre-existing contracts with school districts had already identified the Equitable as the underwriter of the group policy. In response, MESSA decided that all MEA local affiliates receiving MESSA coverage had to negotiate the change in underwriters into the contracts with their employers. Without the contractual consent of both parties, MESSA would not change the underwriter to Blue Cross until the next contract renewal period. This action contradicted the precedents of 1964 and 1976, when MESSA unilaterally changed the underwriter of its health insurance plans without the consultation or consent of either its members or its customer school districts.
A notice distributed by MESSA to its members entitled Information Concerning MESSA Health Plans explained MESSA's initiative to involve itself in contract negotiations. The section entitled "Changing From A MESSA/Equitable Plan To A MESSA/Blue Cross Plan" stated in part:
It will be the policy of MESSA that all Super Med plans will continue to be underwritten by Equitable until such time as we receive written notification requesting a change from an Equitable underwritten plan to a Blue Cross underwritten plan. Where MESSA health coverage is provided through a collective bargaining agreement, the written notification to MESSA must be signed by representatives of the employer and the employee group, union, or association. 28 [Original emphasis]
The proposed change in underwriters was to reduce the premium rates previously charged to school districts, since Blue Cross coverage was less expensive than similar coverage from the Equitable. As an incentive to change immediately, MESSA promised school districts that it would waive the rate increase for Equitable plans if districts switched over to Blue Cross. The total cost savings for each district after the change to Blue Cross amounted to 12 percent of premium cost, based upon MESSA's figures .29
If school districts would benefit from the cost savings, then why wouldn't MESSA allow the districts to consent to the cost savings without further negotiations with the union? Furthermore, why did MESSA suddenly decide that it needed the permission of both its members and customer school districts before it could change underwriters when it never needed such consent in the past? The full context of this situation best serves as a clear example of how MESSA can directly impinge upon the collective bargaining process with school districts.
According to testimony provided by Warren Culver, MESSA's current executive director, MESSA felt that local teachers' unions should be given the chance to negotiate new deals with their employer school districts, because new negotiations would provide an excuse for the local unions to seek out additional benefits.30 In fact, many local bargaining units made potential cost savings conditional upon new contract negotiations with their districts. These local bargaining units demanded that the school districts pass along all or part of the cost savings to employees in the form of higher wages or additional benefits. Allegations contained in a charge filed with the Michigan Insurance Bureau in 1985 contend that the MEA, rather than MESSA, ordered this policy.31 Furthermore, it was alleged that the MEA, MESSA, and MEA local bargaining units had discussed strategies whereby MEA locals would attempt to recover premium savings from school districts.
The apparent good-faith intentions of MESSA to include school district input into a major policy decision turned out to be a ploy whereby MESSA would promote the interests of the MEA and its local affiliates by providing another opportunity to negotiate additional benefits. School ' districts were faced with a choice between staying with the Equitable and paying higher premiums, or switching to Blue Cross, paying lower premiums, but having to reopen contract negotiations.
The practice of a union trying to force school districts to share cost savings with union members could be called a vague form of coercion. Beverly Wolkow of the MEA reinforced this possibility in the May 24, 1986 edition of The Voice, when she wrote, "Our conversion to Blue Cross as an underwriter put $20 million in health care savings into other increased benefits in local contracts."32 While trying to pass off a change in underwriters as a favorable reduction in premium costs, MESSA, working on behalf of the MEA, attempted to absorb the cost savings from school districts by increasing the benefits in labor contracts.
It may seem unreasonable to criticize MESSA based upon this single example; nevertheless, school districts have testified that MESSA field service representatives have a prominent advisory role during contract negotiations. In many instances, the school district's bargaining team has found a MESSA representative seated with the MEA's bargaining team during the negotiations. The MEA's own documents have shown that MESSA field representatives actively collaborate with its bargaining representatives, such as one guideline instructing bargainers to "involve MESSA in meetings where bargaining guidelines are established."33
Competitive bidding is an essential part of every school district's budgeting process. A choice of purchasing options allows a school district to locate the most cost-effective supplier. The district can make cost/quality comparisons and contract with those firms which best suit its needs. According to the state of Michigan, public school districts must acquire competitive bids for most purchases costing more than $13,557.34 At the same time, the selection of insurance administrators major expenditure in every district's budget - is a mandatory subject of collective bargaining, rather than a free-market business decision. And when a collective bargaining agent has a vested interest in a certain insurance administrator, the market is effectively closed. In almost every instance where competitive bidding has been successfully utilized, the public interest has been served because school districts have minimized expenditures and maximized quality of service. Without competitive bidding, as in the case of negotiated administration of insurance benefits, there is no guarantee that the chosen firm will perform up to any standards of efficiency. This is one of the main problems with MESSA.
Public school employees have always been concerned that a move to competitive bidding of their insurance would cause a reduction in their benefits. This is simply not true. School districts would still have to negotiate the level of benefits with the union, and the bidding process would be based upon the corresponding level of negotiated benefits. Any change in the amount of employee benefits would be conditional on the union's consent during the collective bargaining process. In any event, with the exception of the MEA, competitive bidding would function in the best interest of everyone involved, including public school employees.
MESSA operates in a market where the insurance administrator that gets the business is the insurance administrator that was negotiated with the most tenacity. This does not necessarily entail that the negotiated insurance administrator is the most efficient firm. The government is paying MESSA to do something that other firms could do more efficiently, if given the chance to compete, but MESSA has the support of the teachers' union. Any form of monopoly or oligopoly-union enforced or otherwise-in a marketplace where public sector firms shop is not going to function in the public's best interest, because nothing compels firms to price competitively. If competitive bidding were implemented, there would be an assured cost savings.
According to the Senate Majority Policy Office, the total potential cost savings from requiring competitive bidding of public school employee insurance is estimated at $60 million." In other words, because the state of Michigan does not permit school districts to select the most cost-effective administrator of insurance without regard to the MEA, school districts are throwing away $60 million. It is important to remember that this is not an immediate cost savings, but one which must be given time to emerge. Before any savings can be realized, competing insurance administrators will need to acquire some knowledge of the risk involved with insuring public school employees. At the present time, MESSA owns the rights to this knowledge as it pertains to MESSA's members. Nevertheless, the state is ignoring a cost containment strategy worth millions of dollars, which could be put to good use in light of the recent debate over funding for public education.
The impediment to the $60 million in cost savings is the court decision that has prevented school districts from competitively bidding their employee insurance coverage. The only way this decision can be overruled is through legislative action. In the past, several initiatives have been proposed in the state legislature which would mandate competitive bidding of insurance in school districts, but none have gathered sufficient support. In an October 5, 1993 speech on school finance reform, Governor John Engler repeated the call for competitive bidding of insurance as one way to alleviate the "budget crunch" in public education. The only hope for school districts is that legislative action will eventually garner enough support to loosen MESSA's grip on the market for administration of insurance benefits to public school employees" giving other more efficient firms a fair chance to compete for school district contracts.
In 1991, the House Fiscal Agency reported that health insurance costs for public school employees rose 801 percent over the previous decade.36 By comparison, expenditures for state employees’ health insurance rose 269 percent over the same period. The rising cost of health insurance in general can be attributed to any number of factors: inadequate reimbursements for Medicare and Medicaid, expanded ranges of covered losses, the price of new medical technology, the costs of malpractice insurance, and so on. But why are health insurance costs for public school employees rising at such a rapid rate? The two most obvious reasons relate to the MEA: unionization and MESSA. Since unions such as the MEA historically obtain more insurance benefits from their employers than non-union employees, typical insurance costs among unionized employees are 24 percent higher than average.37 With MESSA, the preexisting high costs are amplified, because the greater than average insurance benefits are purchased from an MEA subsidiary which has secured market predominance through the union's bargaining leverage. There is diminished incentive for MESSA - the largest administrator of insurance benefits to school districts - to economize and minimize the costs of its benefit packages, since a school district's choice of insurance administrator is not based solely upon cost effectiveness. With the MEA demanding greater than average insurance benefits from school districts, and with no need for MESSA to minimize costs in a competitive manner, school districts inevitably will incur higher overall costs for employee insurance.
What is it about MESSA that keeps the costs of its programs so unusually high? For the most part, it is the design of MESSA's benefit packages. In simplest terms, the more insured expenses MESSA is willing to cover, the higher its costs are going to be. Given its purpose of providing the maximum possible benefits to MEA members, MESSA is not averse to accepting higher costs, so long as it can pass them on to school districts. At the present time, the benefit structures of MESSA's most often purchased health insurance plans are extremely generous, covering most health-related expenses in full. Consequently, these benefit levels are driving up the cost of MESSA insurance at a quicker than usual pace. Consider that the average premium for MESSA full family insurance increased at an average annual rate of 15.34 percent between 1986 and 1991, based upon the latest available data.38 Yet in the school employee market as a whole (with MESSA factored in), the average annual increase in premiums was 13.76 percent. For Blue Cross/Blue Shield, the average annual increase was a "mere" 9.63 percent.
And just how generous are the health insurance benefits offered by MESSA? The most frequently purchased MESSA plans are the Super Care and Super Med programs. A sample of the medical expenses covered by these plans includes:39
100 percent of all in-patient and almost all out-patient hospitalization charges,
100 percent of all surgery and anesthesia charges;
100 percent of all in-hospital medical visit charges including pregnancies;
100 percent of diagnostic x-ray and laboratory charges;
100 percent of charges for cancer screening exams and tests;
100 percent of prescription drug charges (Type I plans require a $2.00 co-payment and Type H plans require a $.50 co-payment);
100 percent of home health care charges;
100 percent of human organ transplants including related expenses;
100 percent of allergy testing expenses;
90 percent of miscellaneous medical charges, such as ambulance service, physician office visits, blood transfusions, and prosthetic devices (Type I plans require an annual deductible);
90 percent of out-patient psychiatric treatment.
MESSA also provides a family "stop loss" provision that covers all out-of-pocket medical expenses in excess of $1,000 per year. This is in addition to a $2 million lifetime maximum benefit for major medical expenses. Furthermore, all Super Med and Super Care plans provide additional benefits for life insurance and accidental death and dismemberment.
The cost implications of generous insurance benefits are simple to comprehend. Suppose, for example, that a person was in need of a liver transplant costing $10,000. If an insurance administrator is not willing to cover organ transplants, it will not assume any costs for the operation. Yet if MESSA offers to cover 100 percent of the cost, it must come up with $10,000. MESSA compensates for the additional cost burden of this benefit by spreading it among all customers and adjusting premiums accordingly. It follows that insurance premiums are almost entirely dependent on the expected amount of claims and the anticipated extent of accompanying costs. When cost predictions are high as a result of greater willingness to accept certain claims, premiums are naturally going to be much larger.
Without question, public school employees deserve reasonable insurance benefits. MESSA has made a commendable effort at providing its members with generous benefits, but benefits that are too generous create budgetary problems for those school districts that are actually paying for MESSA insurance. If benefit levels were restructured to a responsible level, premiums rates would decrease, and school districts would save more on their purchase of MESSA insurance. What is a "responsible" level? First off, the public should take notice that the state's employee health insurance program costs $1,000 less per person than MESSA insurance.40 In any event, so long as the insurance now provided by MESSA is diverting huge amounts of public funds away from classrooms, more reasonable insurance programs are certainly worth considering.
Although it is not a unique phenomenon, MESSA insurance premiums have followed a trend of rate increases for the past several years. MESSA does not suggest that its members should help cover the cost of premium increases, but that any increase should be paid by school districts. Past performance also indicates that in those years when MESSA retained earnings from the premiums paid by school districts, those earnings were used to fortify insurance benefits for MESSA members. Even though the money came from taxpayers, MESSA apparently never considered returning it to school districts in the form of lower insurance rates. Hence, school districts are particularly concerned about MESSA's financial performance and the behavior of its insurance premiums.
There are many reasons why insurance premiums rise from year to year. For the most part, premiums fluctuate because of changes in operating costs, inflation, and actuarial predictions of future claims. In the case of MESSA, premiums are rising mostly due to unreasonable benefit designs, but inefficiency in the administration of MESSA insurance plans is also a cause.
Between 1989 and 1992, MESSA's operating expenses increased 32.6 percent, from $20.8 million in 1989 to $27.6 million in 1992. This translates into an average annual increase of 10.9 percent across the three year period. Yet during this period, the number of participants in MESSA insurance programs remained relatively stable and there were no significant changes in benefit structures or operations. Over the same time frame, the consumer price index rose 13.1 percent, or 4.4 percent per year on average. This makes the rise in MESSA's operating expenses more than twice the rate of inflation. The rise in MESSA's operating expenses should not be confused with the typical rapid increase in the cost of health care. In other words, MESSA's operating costs increased without any apparent justification, because there were neither changes of significant consequence to MESSA's insurance plans nor any inflationary factors that may have driven up costs.
Also between 1989 and 1992, MESSA had $95.4 million in operating expenses, or $23.9 million per year on average. If 80,000 people are participating in MESSA health insurance plans and 20,000 receive other lines of insurance through MESSA, the average annual cost of MESSA administration is almost $240 per member. In the competitive private sector, these per participant operating costs are often less than one-third of what MESSA spends. This trend indicates that there has not been a noticeable effort to decrease costs. All things considered, the public should be quite skeptical about increases in MESSA's operating expenses. MESSA has not been very effective in reducing these costs, and school districts must pay the consequences through higher premiums.
Another area of concern for school districts regarding MESSA's financial performance is its accumulation of savings and retention of earnings. According to MEA Executive Director Beverly Wolkow, on the subject of MESSA, "We just aim to break even."42
Yet between 1989 and 1992, MESSA accumulated a net gain of $87 million on revenues of $1.316 billion. In other words, 6.6 percent of MESSA's total receipts during this period were not expended on insurance benefits, but were amassed as surplus income. At the end of fiscal 1992, MESSA had reserves of $74.7 million covering gross premiums of $341.9 million. These reserves may appear to be the equivalent of 2.6 months of claims, but MESSA does not use them to pay for any claims! Blue Cross maintains a separate insurance reserve for MESSA that is used to cover claims resulting from unusual losses or bad experience.
With this kind of financier reserve, MESSA has several options. It could increase either the covered cost percentage of benefits or the actual quantity of benefits provided. MESSA could also use the reserves to stabilize rates whenever Blue Cross attempts to recover a significant loss resulting from abnormal utilization of benefits. It can use reserved funds to level out premiums among school districts, so districts with good experience ratings subsidize those with poor ratings. Or, when MESSA quotes insurance rates for school districts, it can "low ball" the initial price and make up any difference through higher premiums in subsequent years. Regardless, MESSA is taking in more money than it is spending, and a portion of the public funds that MESSA receives from school districts is accumulating as retained earnings.
Furthermore, MESSA has over $100 million in the form of cash, cash equivalents, investments, and receivables. Approximately $74.7 million of this reserve can be applied as a surplus, or the aforementioned "reserve." And while MESSA will argue that this money is an insurance reserve, nothing prevents MESSA from applying it to any expenses. For example, if any effort was initiated by a public body to hinder the future operation of MESSA, this fund could be tapped to finance the opposition. MESSA might do well to keep only the necessary amount of reserve funds for expenses such as product modifications, and then return the excess money to customer school districts in the form of premium reductions. Nothing presently compels MESSA to give any surplus public funds back to school districts, even when the additional funds are a blatant excess.
It is important to distinguish between the design of MESSA's benefits-the type of coverage provided-and MESSA's cost of administering those benefits. For the design of the benefits contained within MESSA health insurance plans, MESSA's total cost of providing the benefits can be among the lowest available. One reason for this is that benefit costs decrease as the size of purchases increases. In other words, MESSA has produced an economy of scale by representing in excess of 80,000 participants.
Because of this, MESSA can be competitive with other insurance providers, even though MESSA's administrative costs are unusually high. Specifically, MESSA's total administrative expenses are around 13 percent of annual premiums, when most TPAs have administrative costs equal to 4 or 5 percent of annual premiums. The economy of scale resulting from MESSA's group size obscures the fact that there are significant savings to be had in reducing administrative costs.
When MESSA published its premium rates for 1993, the rates were typically lower than similar rates charged by Blue Cross--which competes against MESSA, as well as underwrites its coverage--for the second plan year in a row. This phenomenon is somewhat ironic, because for the plan years prior to 1991-92, MESSA insurance was considerably more expensive than Blue Cross insurance. Some school districts have been led to believe that they are actually receiving a good deal from MESSA. The Saginaw School District, for example, chose direct Blue Cross coverage in 1990 and saved over $1 million per year compared with MESSA. Even though the insurance benefits were not entirely comparable to MESSA, the District and the Saginaw Education Association agreed to the package. According to testimony before the House Appropriations Committee, the monthly cost of full family coverage for a teacher in the Saginaw School District was $442.69 through MESSA .43 Coverage purchased directly from Blue Cross would have cost $299.25. In June of 1993, the Saginaw District became a MESSA customer when Blue Cross premiums rose 22 percent from the previous year, costing the District an additional $600,000 over MESSA coverage.44 Even though MESSA has now become less expensive than Blue Cross for reasons that are not immediately clear, school districts must weigh the short term benefits against the long term costs.
While it is generally more practical to purchase the less expensive plan, school districts cannot afford to let prices deceive them. Lower rates do not pardon the waste of MESSA insurance programs. There is savings in the short run, but there could be even more savings if MESSA provided more efficient benefit packages and was more mindful of school district budgets. In addition, school districts must remember that MESSA has substantial cash reserves and investments which would allow it to subsidize premiums at a rate lower than Blue Cross even if MESSA actually cost more than Blue Cross. MESSA could also charge more in one school district in order to charge less in another. Some have speculated that MESSA is not cheaper in the long run; that MESSA is allegedly enticing districts with low initial rates, only to hike up the rates once its insurance plans are secured by contracts. In addition, school districts can often become locked-in to MESSA insurance. The process for arranging new coverage outside of MESSA is tedious and difficult, and often times impossible. Public school employees have demonstrated a willingness to accept reduced wages in order to maintain MESSA coverage.
School districts must accept their fair share of the responsibility for the impact of MESSA on the cost of public education, as long as they continue to acquiesce to the excessive employee insurance benefits provided by MESSA. While several school districts have, vocally expressed reservations about MESSA, many districts are culpable to the extent that they have failed to effectively combat MESSA. For example, a prime reason costs for school districts have increased is that districts often negotiate the design of benefits provided to their employees by making comparisons to neighboring school districts. But if neighboring school districts also purchase MESSA insurance, then of course school districts will obtain inflated comparisons of benefit designs in similar districts. A more objective basis of comparison would be the benefits offered by similar employers in the school district's region.
Part of the reason for the acquiescence of many school districts to MESSA is the influence of the MEA. In the vast majority of districts, superintendents and business managers maintain control over district operations. Many of these officials are former teachers and therefore former members of the MEA. The MEA cultivates these relationships and enjoys the favor of many district officials. Consequently, there are very few strong superintendents with the willingness to resist MESSA and the MEA.
At the present time, around 23 percent of the average school district's operating budget is allocated for employee insurance benefits.45 With this drain on the financial resources of school districts, there is legitimate concern that the rising cost of MESSA coverage will force many school districts to cut educational programs. As costs rise, school districts must either turn to the taxpayers for additional funds or reduce the level of educational programs. The Michigan Association of School Boards, which favors the idea of maintaining current benefit levels so long as they are provided more efficiently than MESSA, noted this problem:
If schools cannot control the cost of health insurance coverage, it will take an increasing portion of every school's budget. This means there will be fewer dollars left to maintain andlor improve current programs. Health insurance premiums are rising at a rate of 11 percent to 12 percent per year-school budgets are increasing at a much slower rate. 46
According to data provided by the MASB, the average annual cost for full family health insurance coverage is approximately $5,700. In the year 2000, that same cost is expected to be $14,170-an increase of 148.6 percent. Unless school district revenues rise by an equal amount, health insurance expenditures will require an even larger proportion of school district budgets. Realistically, there is little chance that enough tax revenue will be acquired to increase school health care budgets by 148.6 percent.
With employee compensation increasing and taxpayers more resistant than ever to additional funding proposals, it is apparent that school districts will have to make budgeting changes. Districts could eliminate positions, but the threat of union resistance is too much to bear for most districts. Another alternative is to roll back or eliminate programs. In the worst case scenario, the school district could shut down altogether, as the Kalkaska schools did in March of 1993 when citizens rejected a tax increase and the district could no longer afford to operate. Or, perhaps, school districts could make some targeted effort at controlling the cost of employee insurance, which would entail a frontal assault on MESSA.
For the time being, MESSA enhances the overall problem by charging school districts high rates for health insurance while cost-cutting options remain untapped, such as the option of moderating benefit levels. MESSA will contend otherwise, but when it has $100 million in available cash and cash equivalents, there is no way of evading the issue. As long as taxpayers are hostile to millage proposals and tax increases, MESSA's insurance premiums continue to rise, and MESSA receives public funds in a noncompetitive market with only minimal incentives for improving efficiency, school districts will have to pay for higher employee insurance at the expense of other educational programs.
Any discussion of MESSA cannot neglect the role of the health care corporation which underwrites the majority of MESSA's business: Blue Cross/Blue Shield of Michigan ("Blue Cross"). Now that MESSA and Blue Cross have a commercial affiliation by virtue of an underwriting agreement, there is relatively no competition among underwriters for health insurance administration to educational employees. As shown in Appendix II, Blue Cross, has acquired a dominant share of the market by contracting directly with school districts or by underwriting all of MESSA's group policies.47 According to Blue Cross's corporate headquarters, MESSA is one of its largest accounts, although it would not specify how large. Given this degree of interest, Blue Cross will almost certainly defend MESSA against criticism and oppose any attempt to regulate MESSA's operations.
From time to time throughout its 33-year existence, MESSA has recruited new underwriters for certain insurance plans in order to keep pace with varying market conditions. In response to the escalating cost of health care throughout the mid-1980s, MESSA sought alternative delivery systems for its health insurance plans. The search for a new system concentrated on MESSA's desire to control charges for medical services while preparing for future trends .48 After months of deliberation, MESSA decided in 1985 that a business arrangement with Blue Cross would best serve its needs.
For nearly 25 years prior to this, MESSA and Blue Cross had competed vigorously in selling health insurance to public school employees. While the Equitable Life Assurance Society was still underwriting MESSA's health plans, Blue Cross was offering lower prices to school districts for similar coverage. Unable to beat the competition, MESSA joined it, and a confidential operating agreement was formed between Blue Cross and MESSA.
The underwriting arrangement with Blue Cross is organized in such a way that MESSA is able to design the benefits of each plan. Once the plans are established, they are consigned to Blue Cross for underwriting purposes. Blue Cross calculates the assumed risk of the plans and charges MESSA for the protection. Even though Blue Cross underwrites the plans and guarantees coverage, MESSA retains the predominant share of administrative responsibilities. Although this arrangement does not violate any law, it does not function in the public's best interest, because it entails unnecessary costs that result from poorly designed benefit structures.
Third party administrators such as MESSA which administer insurance benefits that are underwritten by commercial carriers must enter into an agreement for underwriting services with a licensed insurer. Aside from underwriting specifications, the agreement between the administrator and the insurer of the benefits identifies the arrangements for payment, administration, filing of claims, etc., and delegates various tasks. While responsibilities may vary from agreement to agreement, the underwriter always provides the actual coverage and charges a corresponding rate to the administrator. The administrator, whose name is usually on the insurance plan, then bills its members or their employers for the combined cost of administration and underwriting services.
The various provisions of the cooperative venture between MESSA and- Blue Cross are detailed in an operating agreement dating back to August 13, 1985. Pursuant to this agreement, MESSA is actually administering Blue Cross insurance to public school employees under the MESSA name. Blue Cross assumes full risk for paying the benefit costs associated with MESSA health plans (unless those costs are outside of the scope of the agreement). MESSA is responsible for most aspects of administration. Among the more significant tasks allocated to MESSA are:
Calculating and collecting the premiums charged to customer school districts;
Processing applications and enrolling new members;
Issuing certificate booklets and identification cards;
Deciding how any excess revenues will be used;
Identifying eligibility for claim reimbursement;
Adjusting claims and determining the amount to be paid;
Paying certain claims to members;
Overseeing the claims appeal process;
Pre-determining the "reasonable" amounts to be paid for certain claims;
Paying Blue Cross for the cost of underwriting plus a service fee.
The MEA has a stake in the agreement because it maintains control over the structure of benefit packages through MESSA's Board of Trustees. In addition, the MEA takes administrative responsibility for promoting MESSA health plans to its local affiliates and negotiating the plans into labor contracts.
The most essential feature of MESSA's agreement with Blue Cross is that MESSA members are allowed to take advantage of the provider arrangements that Blue Cross has with hospitals, physicians, and other health care providers in the state of Michigan. This arrangement permits MESSA to procure the special discounts that Blue Cross receives from its participating health care providers. Participating providers agree to accept slightly lower payments in exchange for a guaranteed volume of business. These special discounts are advantageous to customer school districts because participating providers cannot overcharge MESSA for services, thereby limiting the overall cost of MESSA plans.
The discounts are also an effective cost-reduction mechanism for MESSA members. Participating providers in the Blue Cross/Blue Shield program have agreed in advance to accept the "reasonable and customary" payment for medical services, as determined by Blue Cross, and to receive direct compensation from Blue Cross for any services rendered to MESSA members. MESSA members do not have to worry about being overcharged or compensating for any difference that would result if a provider charged above the "reasonable and customary" level. Yet, even if this arrangement did not exist, MESSA would most likely accept the burden of excess charges on behalf of its members as part of its goal to reduce their personal liability for costs.
Despite the agreement with Blue Cross, nothing compels MESSA members to receive medical services from Blue Cross participating providers; members also have the option of receiving treatment from providers that are not affiliated with Blue Cross. Non-affiliated providers may participate on a case-by-case basis, but only if they agree to accept Blue Cross's terms of payment. Like regularly participating providers, nonaffiliated providers who agree to participate submit their claims directly to Blue Cross using the standard Blue Cross filing system.
In the other situation, where the provider is neither affiliated with Blue Cross nor willing to participate with Blue Cross in the particular case, the MESSA member can still receive treatment and send the itemized invoice to MESSA, rather than Blue Cross. This type of claim is processed by a MESSA employee and paid according to MESSA's own "reasonable and customary" fee schedule using a MESSA check. Although Blue Cross has determined a schedule of reasonable charges for health services, MESSA is allowed to disregard this schedule when handling certain claims. Blue Cross has no other contract arrangement quite like this.
MESSA contends that its operating agreement with Blue Cross is so confidential that it will not disclose any information about the contents to its members, customer school districts, or the taxpaying public. MESSA will only allow the Insurance Commissioner to examine the agreement for investigative purposes, and it will not let the Insurance Bureau retain a copy. A letter from MESSA's attorneys to the Insurance Bureau best summarizes the secrecy of this agreement:
MESSA and Blue Cross have gone to substantial lengths to preserve the confidentiality of their trade secrets. MESSA will vigorously oppose public disclosure of these confidential trade secrets… Public disclosure of the trade secrets is not necessary and will not serve the public interest.49
To the contrary, disclosure of the agreement would serve the public interest by allowing citizens to scrutinize the efficiency of an operation which is funded by public school districts. Information obtained through interviews and public records demonstrates that the operating agreement does contain inefficiencies affecting MESSA's design of benefits, which work to the advantage of MESSA and Blue Cross, but are wasteful from the public's point of view.
To the detriment of public education, MESSA has created inefficiency and waste in the administration of health insurance. First of all, even though one system for the processing of claims could accommodate both MESSA and Blue Cross, two separate systems have been established in order to give MESSA members more choices for health care. In addition, MESSA encourages unnecessary costs by not taking reasonable measures to control utilization of certain programs. The combined effect of these deficiencies is higher costs and less money for school districts.
Prior to its operating agreement with Blue Cross, MESSA processed all claims submitted by its members. When MESSA contracted with Blue Cross in 1985, the claims processing systems of both corporations were integrated using a complex computer network. A common history file was developed, which lists the record of claims for each MESSA member. Each time a claim is received, either by Blue Cross or by MESSA, the data is entered into this common file. And while the history file may be common, the data entry system is not. Blue Cross and MESSA each maintain separate operations for the processing of claims.
Whenever a MESSA member receives treatment from a participating Blue Cross provider, the claim is processed by Blue Cross. Yet, whenever a MESSA member is treated by a non-participating provider, the claim is processed by MESSA. There is no need to have two separate facilities entering data into one file-a duplicated filing system. Even though MESSA could arrange to have the claims processing aspect of administration centralized into a single operation, it needlessly continues to process certain claims. For example, MESSA could have all claims forwarded to Blue Cross and entered into a single history file. Even if a provider is not participating with Blue Cross, that does not automatically disqualify Blue Cross from handling the claim. Blue Cross, however, has the facilities and capability of handling a large volume of claims, so any additional costs would be marginal in this case. MESSA could then reduce expenses by minimizing the cost of claims administration and scaling down the magnitude of its computer network.
Why doesn't MESSA let Blue Cross process these claims just as any other third party administrator would? With its other accounts that are similar to MESSA, Blue Cross consistently works off of one centrally organized history file. Yet, MESSA is granted an exemption from standard practice because MESSA believes that it is protecting its members from any disregard that Blue Cross might have for their financial interests while claims are being processed. Furthermore, Blue Cross accepts without question the payments made by MESSA to MESSA members for relevant medical expenses. Blue Cross takes these payments for granted and builds them into its rate structure. In other words, Blue Cross does not arbitrate or verify MESSA-incurred benefit costs which will be passed along to school districts in the form of premiums for health insurance. This would not seem to be responsible behavior for a quasi-public corporation created to serve the public interest.
The estimated waste of this duplicate filing system extends into the millions of dollars, based upon the expenses for data processing listed in MESSA's "Schedule of Operating Expense."50 One estimate places the waste of duplicate administration at around $27 million.51 But if this procedure is clearly wasteful, why wouldn't MESSA take corrective action? Consider what would happen to the MEA if MESSA's operations were streamlined.
Remember that both MESSA and the MEA contract with MEDNA for data processing services. In actuality, MESSA is paying MEDNA to operate the computer network which is at the core of claims processing. If MESSA operations were relinquished to Blue Cross, there would be little need for MEDNA to maintain its vast data processing resources. Since the MEA depends on MEDNA for access to MESSA's computing resources, the MEA would suffer a blow if MEDNA were pushed out of business.
If MESSA were removed as a co-administrator of its health insurance program, the immediate savings could exceed $20 million in administrative expenses, and millions more in controlling fees paid for physician and ancillary services. In 1992, MESSA had a composite premium obligation of $327 million to its underwriters. If $300 million of that total was owed to Blue Cross, and if Blue Cross had standard administrative expenses of 7.5 percent excluding charges for insurance reserves, the total Blue Cross administrative charge to MESSA in 1992 was $22.5 million. The $27.6 million in operating expenses listed in MESSA's financial statements does not include expenses incurred by Blue Cross. If .$20 million of this amount was to co-administer Blue Cross insurance, then the total administrative expense for MESSA health insurance was $42.5 million, or 12.75 percent of premiums. For a third party administrator, this expense is typically around 4 or 5 percent, and rarely will it ever exceed 7 percent. If even reduced to the 7 percent level, the annual savings for 1992 would have been $21.5 million.
Another factor that contributes to the cost of MESSA's health programs is its offer to pay for services rendered by providers who do not participate in Blue Cross. Although access to non-participating providers is an added benefit to the members, MESSA could reduce costs simply by limiting the options given to members for receiving medical services, as many managed care programs do. While members can reduce costs by patronizing only participating Blue Cross providers, there is neither a requirement nor an incentive for them to do so.
As previously noted, whenever a MESSA member receives care from a participating Blue Cross provider, Blue Cross minimizes costs for MESSA by compensating the provider based upon a discounted fee schedule. However, in cases where a MESSA member is treated by a provider that refuses to accept Blue Cross's payment, MESSA receives the bill from the member, processes the claim, and reimburses the member. (MESSA deducts any amount paid to its members from the total amount that it owes to Blue Cross, so Blue Cross is still at risk, since MESSA does not pay for any claims which exceed its premium obligation to Blue Cross.)
The actual reimbursements for medical services are based upon MESSA's determination of how much the service is worth. In 1985, MESSA claimed that its schedule of "reasonable and customary" fees was similar to the one used by the Equitable.52 In fact, the reimbursements offered by the Equitable are larger than those offered by Blue Cross. Regardless, MESSA's valuation of reasonable fees is inflated above Blue Cross's valuation of reasonable fees. But for what reason?
Suppose a MESSA member can receive the same service from a participating provider or a non-participating provider, and MESSA will cover 90 percent of the cost up to the reasonable and customary level as determined by the processor of the claim. The participating provider is limited in how much it can charge, since it will only receive the reimbursement that Blue Cross has determined to be reasonable. The non-participator can charge more for the same service, because Blue Cross does not set its prices. Since MESSA is aware that non-participators will charge a higher rate to its members than participating Blue Cross providers, it has set inflated determinations of "reasonable and customary" charges in order to limit out-of-pocket expenses for its members. In this sense, non-participators can "balance bill" with MESSA's fee schedule. From a practical standpoint, it is in the best interest of all providers not to participate with Blue Cross when treating a MESSA member in order to overcharge the member and let MESSA pickup the costs.
According to its 1992 financial statements, MESSA itself spent a total amount of $14,168,617 on direct benefits paid to members, which would include payments to members who chose to receive medical services from non-participating providers. MESSA could avoid any excess costs by using a deflated fee schedule, or it could eliminate them altogether by requiring its members to patronize only participating Blue Cross providers.
There are other ways MESSA can improve the efficiency of its arrangement with Blue Cross, specifically through "managed care" initiatives. A study conducted by the Rand Corporation found that 20 percent of national health care expenditures is consumed by unnecessary use of services.53 With MESSA, there are few managed care incentives that encourage members to use less health care services, so overuse of MESSA programs is expected to be much higher than average. For example, although this practice contradicts standard Blue Cross procedures, Blue Cross does not require that MESSA members obtain verification from Blue Cross before checking into a hospital. Pre-admission certification, as it is called, can reduce costs by eliminating unnecessary hospital stays. Yet, MESSA has kept all of its utilization review programs in-house in order to protect its members from unfavorable cost arbitration. MESSA members are given the option of having a MESSA Care Rider, which requires pre-admission certification for in-patient hospital treatment, second opinions for surgical procedures, and medical case management. The Care Rider reduces costs billed to the member by five percent.54 If MESSA mandated that all members have this Care Rider, MESSA would be able to avoid certain needless medical expenses and reduce overall costs.
According to the Health Insurance Association of America, in 1990, only five percent of group health insurance plans offered unlimited choice of physicians and no control over the use of medical services.55 While some will argue that MESSA is among the five percent, and others will argue that MESSA does manage care to a certain extent, the fact remains that MESSA's managed care measures are minimal when compared with the measures undertaken by other insurance administrators. As long as MESSA members anticipate that most medical claims will be covered in full, they believe that MESSA will always interpret policies in their favor, and they are not forced to pay many out-of-pocket expenses, there is little incentive to restrict overuse. MESSA could implement a managed care program of cost sharing, selective contracting, and utilization review that would dwarf its current program, yet still be fair to its members. The typical potential savings with various managed care options are estimated as follows:56
Deductibles: 10 percent of premium.
Co-payments: 5 percent of premium.
Employee premium contribution: 5-8 percent of premium.
Coordination of benefits (to assure that the employer's insurance is primary): 7-10 percent of premium.
Utilization review (assure acute days and aggressive discharge planning): 10-15 percent of premium.
If MESSA could even reduce premiums of $300 million by just 10 percent through managed care measures, the savings would be $30 million. This is certainly possible. In the past, MESSA has contended that it does use managed care. Again, MESSA's use of managed care is not sufficient to limit noticeably the costs of MESSA's benefit packages. As of late, there have been persistent rumors circulating that MESSA is now actively exploring managed care initiatives in response to the Clinton health care reform proposals. What remains important is that if MESSA ever does implement a managed care program, it must be effective and not just a token act if costs are ever to be reduced.
The wasteful and costly provisions of MESSA's operating agreement with Blue Cross are based upon the overall design of MESSA health insurance plans, and not some callous intended effort to raise costs. The way any potential savings can be realized is by modifying the design of MESSA benefit packages. Yet, the design of MESSA's benefit packages can only be changed through MESSA's own initiative, a legislative requirement, or the collective bargaining process between school districts and the MEA. Nevertheless, if administrative expenses were minimized and managed care was implemented so as to reduce costs by just 10 percent, the total potential savings of cleaning up MESSA's health insurance program is estimated at a minimum of $50 million.
Recently, there has been some confusion over MESSA's role as a risk taker. If MESSA paid for certain claims outside of what it owed to Blue Cross, then it would qualify as an at-risk insurer rather than an administrator. There have also been questions about the legality of MESSA because MESSA would be violating the insurance code if it accepted risk in its insurance plans. MEA Executive Director Beverly Wolkow has testified that MESSA does share risk with Blue Cross.57 But this contradicts a previous MESSA statement explaining, "These are fully insured/underwritten contracts. MESSA takes no risk."58 All things considered, MESSA technically does not appear to have accepted any explicit risk. Yet, this does not mean that MESSA is absolved of any implicit risk.
The implicit assumption of risk can be found in the formula which calculates the underwriting results that are to occur if MESSA ever terminated its contract with Blue Cross.59 The ultimate risk taker for MESSA health insurance plans is Blue Cross, but this insured risk must be put in its proper perspective. Blue Cross's ultimate risk for MESSA health insurance plans is limited to a reserve deficit in excess of 10 percent of annual premium but only at the time the MEA cancels the operating agreement. If Blue Cross suddenly stopped underwriting MESSA plans, it would still be liable for claims which have been incurred but not paid as of the termination date. The operating agreement dictates that Blue Cross will establish a Rate Stabilization Reserve (RSR) in order to cover these claims-in-process in the event that the operating agreement is ever canceled. The accumulated underwriting results of all prior ratings periods are debited or credited to the RSR. If the MEA cancels the agreement, all claims have been satisfied, and the balance in the RSR is positive, the leftover money is refunded to MESSA. If the balance is negative, Blue Cross recoups the difference from MESSA. The ultimate risk of Blue Cross to pay for claims-in-process is confined to any amount over 10 percent of the annual premium it receives from MESSA.
Suppose, for example, that MESSA paid $300 million in premiums to Blue Cross last year. Also suppose that last year, MESSA canceled its underwriting agreement with Blue Cross. Up to that point, any of MESSA's premium payments to Blue Cross that were not used to pay for' insurance benefits during the applicable plan year were added to a cash reserve. Similarly, any losses during a plan year were deducted from this reserve. At the time MESSA canceled its agreement with Blue Cross, the balance in the reserve totaled $45 million. If any claims remain unpaid at the time the agreement is canceled, MESSA has to pay for the first $30 million worth of claims, or 10 percent of annual premium. Blue Cross must come up with the difference of $15 million. In the opposite situation, if there were no unpaid claims at the time of cancellation, Blue Cross would keep $15 million and refund the $30 million to MESSA-a windfall profit.
The likelihood of a reserve deficit exceeding 10 percent of premium at the time the agreement is canceled is so remote that the operating agreement between the parties resembles more of a "minimum-premium" or "self-funded cash flow" arrangement. Under such an arrangement, MESSA would anticipate its future claims and reserve just the right amount of funds to meet the contingencies. Right now, the rate structures charged to MESSA by Blue Cross practically guarantee that enough money will be generated to cover MESSA's benefit costs for the year. If the rates generate more than enough money, the surplus is deposited in a reserve. The only time there would be any practical risk for Blue Cross is when the underwriting agreement is canceled and the cost of unpaid claims exceeds 10 percent of last year's premium, because that is the only time when the actual "insurance" will kick in. The entire risk is born by Blue Cross, but the practical risk for Blue Cross is minimal to non-existent. Realistically, Blue Cross would only be at considerable risk if MESSA somehow refused to make payment.
Besides the waste and high costs which have resulted from MESSA's operating agreement with Blue Cross, there are several other concerns about MESSA's relationship with the underwriter of its health insurance plans. Specifically, these concerns pertain to the possible unfair trade practices which may have resulted from MESSA's financial affiliation with Blue Cross.
Some may wonder if MESSA's contract for underwriting services from Blue Cross is less of an operating agreement and more of an agreement to restrain trade. After all, the most noticeable consequence of the joint operations is that MESSA and Blue Cross now control the dominant share of the market for administration of health insurance benefits to public school employees. Questions about restraint of trade are also justified when considering the non-standard aspects of the operating agreement. For example, according to testimony provided by the Michigan Association of School Boards:
Another problem with the MESSA/BCBS relationship is that BCBS gives MESSA access to discounts with hospitals and other health care providers, negotiated by BCBS, based on the massive amount of total business it controls. There would be no objection to accessing this discount except BCBS apparently is unwilling to offer other health insurance companies, which compete with MESSA, the same access to its buying power. When another insurance company recently sought the same arrangement MESSA had, BCBS offered only a different, less desirable agreement.60
There are several factors that suggest possible improprieties in the relationship between MESSA and Blue Cross which would adversely affect competing firms within their market.
Interlocking directorates are sometimes referred to as "per se" violations of antitrust law-their mere existence is intrinsically offensive.61 Interlocking directorates occur when a person serves as a director in two or more competing corporations. As this definition applies to the arrangement between MESSA and Blue Cross, an interlocking directorate is now present. Charles Neumann, the President of the MESSA Board of Trustees since 1976, is also a member of the Board of Directors for Blue Cross/ Blue Shield of Michigan. MESSA cannot argue that it does not fit the definition of a "competing corporation" with Blue Cross, because MESSA has denied previous unfair trade practice allegations by contending that it competes vigorously with Blue Cross.
The problem is clear: federal antitrust laws grant exemptions to the business of insurance, and Michigan's antitrust laws provide additional exemptions to insurance related businesses which are already subject to other state regulations.62 It is not readily apparent that there is any legal offense to the MESSA/Blue Cross interlocking directorate, because, their operations are exempt from antitrust laws. Moreover, it is not uncommon for Blue Cross to have its larger corporate customers participate on its Board of Directors. At the same time, it is not common for Blue Cross to have its corporate competitors represented on its Board. Nevertheless, there is speculation that MESSA exercises undue influence over Blue Cross through the interlocking directorate involving Mr. Neumann.
A most recent example of this speculation involves a conflict between Blue Cross and one of MESSA's fiercest competitors-the School Employees Trust ("SET"). In 1992, as part of a strategy to expand benefit programs while reducing costs, SET petitioned Blue Cross for "sponsored organization" status-the same status given to MESSA-but the request was denied. As a "sponsored organization," MESSA receives certain privileges from Blue Cross that are not available to MESSA's competitors such as SET. For example, MESSA obtains preferential rates from Blue Cross because its experience ratings are based upon its own claims history. SET's ratings, however, are based upon the claims history of the entire education industry grouping. Without the similar consideration given to MESSA, competitors cannot offer similar coverage to their members. When the attorneys for SET demanded that Blue Cross provide an explanation of this denial, Blue Cross said the decision was in the interest of 6 1 maintaining fiscal and underwriting stability:"
SET has coverage available to its members. While the specific coverages available through MESSA are not offered, BCBSM is not required to offer all programs to all groups.63
In a letter to the Insurance Commissioner, the attorneys for SET noted their skepticism about Blue Cross's arrangement with MESSA by stating: "This denial... constitutes a restraint of trade by competitors of SET represented on the Board of BCBSM."64
One extension of the argument claiming that MESSA maintains inappropriate control over Blue Cross is the common allegation that both corporations actively collude. Charges of collusion are serious, and if they can be proven, they would most likely constitute a restraint of trade. While third party administrators are common in the insurance industry, it is not common for a third party administrator to be underwritten by a major competitor. Ever since MESSA and Blue Cross began cooperating pursuant to their operating agreement, other competitors in their market have essentially been squeezed out. And given the experiences of those who deal directly with MESSA and Blue Cross, the speculation about collusion is understandable.
The Assistant Superintendent of the Clawson School District, for example, analyzed the trends of premium differentials between Blue Cross and MESSA coverage.65 He observed that MESSA coverage was historically more expensive than Blue Cross, but MESSA's rates abruptly became less expensive during which time MESSA claimed that it was having problems with a disproportionate number of claims and while Blue Cross rates jettisoned upwards. He suspects that MESSA colluded with Blue Cross to raise Blue Cross premiums so school districts could no longer argue that Blue Cross was cheaper than MESSA. Whether MESSA is the plan name or Blue Cross is the plan name, the business of underwriting still goes to Blue Cross.
A similar situation occurred during the Troy School District's 1990 contract negotiations (discussed with details in Appendix III). A Blue Cross representative provided the District with quotes for health insurance rates. Although the District reviewed the quotes on many occasions with the Blue Cross representative, the quotes were never documented in writing. One week before the start of school, a MESSA representative informed the District that the Blue Cross quotes were wrong. After further consultation with Blue Cross, the District confirmed the accuracy of the quotes. Several days later, Blue Cross informed the District that an error was committed and that the quoted rates would apply only to a select number of teachers, rather than the entire school district.
The original quoted rates from Blue Cross would have saved the District an estimated $700,000. The revised rates would have cost $95,000 more than MESSA coverage. With this sort of behavior, what else can a school district suspect but evident collusion?
But even if MESSA is not colluding with Blue Cross in order to procure a steady market share, MESSA's attorneys remind us, ". . . MEA representatives are good enough bargainers that Blue Cross representatives are aware that schools may choose MESSA over Blue Cross when only one of the two may be selected."66
If the complaints of public school districts serve as any indication, MESSA does not care much about customer satisfaction. And if MESSA's apparent disregard for the fiscal welfare of its customer school districts is any indication, MESSA does not care how its business conduct negatively impacts public education. Why should MESSA care if there is no incentive to care? School districts do not use MESSA because of its cost effectiveness or its exceptional service; they purchase MESSA insurance because the MEA continually pressures them into using MESSA. True, MESSA health insurance is now less expensive than comparable Blue Cross/Blue Shield coverage, but that does not necessarily mean that MESSA is a better buy. It also fails to consider that other private sector insurance companies can provide acceptable service at a more reasonable cost. In fact, MESSA is a far cry from overall quality when considering the abundance of legitimate qualms that school districts have with MESSA.
At MESSA, the needs of members come before the needs of school districts which actually pay for MESSA insurance. Consequently, school districts have experienced several difficulties while transacting business with MESSA which require consideration. These difficulties have severely impaired school districts, because districts are forced to accept additional costs with no practical means of escape. Overall, the problems that school districts have with MESSA have produced an unfavorable business relationship, and MESSA's evident disregard for the situation has fueled discontent about MESSA and the MEA. The problems relate to the failure of MESSA to disclose essential information, to negotiate changes in benefit contracts, and to provide sufficient purchasing options for insurance. Furthermore, school districts have voiced concerns about MESSA's gift coverage program, its requirement of uniform coverage for MESSA PAK insurance, and its decision to eliminate "dual choice."
One of the most recurring complaints made by school districts is that MESSA fails to disclose crucial information about insurance claims which would help school districts target problem areas and develop cost-containment strategies. Specifically, school districts are disturbed that MESSA will not provide them with data identifying the extent of the claims that have been filed by their employees. Without this information, school districts can neither assess the value of their MESSA purchase nor obtain accurate bids from other insurance administrators.
Michigan law mandates that for-profit insurance administrators operating within the state offer information about claims history to their plan purchasers. However, both MESSA and Blue Cross are not-for-profit and covered by a separate law that does not require them to divulge this information. The claims history, or group experience rating, of each school district lets the district know how many medical claims in total were filed by its employees. If this data were available, school districts could present it to various insurance administrators which would review 'the data, calculate the risk involved, and estimate reflective cost of insuring the district's employees. This would be a tremendous step toward allowing competitive bidding.
Without knowing how many claims have been filed by its employees, school districts cannot possibly obtain accurate quotes from insurance administrators. Moreover, there is no way for a district to know if it is receiving a good value in exchange for the thousands of dollars it pays to MESSA for employee insurance. In a letter to the Troy School District, a private insurance agent emphasized the dilemma of not having group experience ratings:
As you can see, it would be difficult for the school district to obtain quotes since your claim experience is not available. In addition, most companies will only quote a self-funded plan. While a self-funded plan will generally save money, we would be unable to determine the amount saved until at least 24 months of claim experience was collected. If MESSA has provided you with any type of annual renewal report which explains their rate action every year, I may be able to more accurately predict the cost of either a fully insured or self-funded plan.67
If school districts cannot verify that similar coverage is available at a lower cost, they cannot convince voting citizens or their employees that they should explore alternatives to MESSA. In this way, MESSA is able to dominate an enormous share of the market for administration of insurance benefits to public school employees.
At the present time, MESSA has structured group experience ratings so they exist according to geographic regions of the state, rather than actual school districts. In other words, a school district could potentially receive group experience ratings, but only for its region, which is not much help. Nevertheless, MESSA will not disclose these ratings. MESSA owns the exclusive rights to the actuarial records for its members, although Blue Cross maintains the records. According to their operating agreement, Blue Cross may not, use this information without MESSA's consent.68
Like all insurance administrators striving to retain a certain market, MESSA is acting out of self-interest by suppressing this information. If the information were disclosed publicly, other insurance administrators would know the risk associated with insuring a group of public school employees. The other administrators would be able to quote premiums for the district and compete with MESSA for the district's money. In a lawsuit filed by school districts seeking to obtain their claims history (which MESSA won), the judge even stated that, ". . . if an employer were to learn its experience was unusually good, the employer could use that information to obtain lower-cost health insurance elsewhere." But for now, school districts are effectively "locked in" to their purchases of MESSA insurance.
When school districts enter into contracts with MESSA for employee insurance, the contracts are the product of an extensive bargaining process. It would seem, then, that any time the contracts are modified, MESSA would have to negotiate the modifications with school districts, and vice versa. This is not the case. MESSA contends that its contracts with school districts are open-ended and revisable at any point during the course of a contract period. Subsequently, MESSA has often made unilateral changes to its health insurance benefit contracts without the consent of its customer school districts. In recent years, for example, MESSA announced in the middle of a contract period that it would begin covering organ transplants. Even though MESSA does not change premiums at the time it, changes contract provisions, it is reasonable to suspect that increased benefits translate into increased premiums over the long run. Regardless, these unilateral contract modifications become a part of a district's health insurance program without any form of negotiation whatsoever, and school districts are justifiably upset.
Many school districts view these actions as duplicitous on MESSA's part because MESSA is not bargaining in good faith. If a school district requested a contract modification from MESSA, then it would have to negotiate with MESSA and accept a rate change.69 MESSA contends that school districts waive their right to object to MESSA initiated contract modifications by signing the "Employer Participation Agreement." This agreement refers to "certificates issued to MESSA" to which customer school districts are bound.70 One of these "certificates" is a summary plan booklet prepared for MESSA members which explains health insurance benefits. On page 48, it states: "MESSA reserves the right to modify or discontinue the group program at any time."71 In accordance with the language of the Employer Participation Agreement, school districts are then bound to inconspicuous statements printed in a MESSA pamphlet.
What is the consequence to school districts of unilateral contract changes? Since the modifications made by MESSA are almost always increases in the benefit structures of insurance plans, school districts suffer the actuarial consequences of benefit increases. Insurance premiums are primarily based upon estimated future claims. If it is probable that MESSA will require additional funds to compensate for utilization of new benefits, then MESSA must either collect the additional funds from school districts in the form of future premiums or remove the additional funds from its cash reserves, which have been financed with previous premium collections from school districts.
MESSA's non-negotiated changes in insurance benefits could become illegal with a recent court ruling in the case of St. Clair Intermediate School District v. Intermediate Education Association/Michigan Education Association and the Michigan Education Special Services Association. On May 8, 1990, during the course of their contract for employee health insurance, MESSA notified the St. Clair ISD that it was raising the lifetime maximum health insurance benefit for members from $1 million to $2 million. In August of that year, the District challenged this action by filing an unfair labor practice charge with the Michigan Employment Relations Commission. The charge claimed that MESSA, as an agent of the MEA, had an obligation to bargain with the District before increasing the benefit threshold, and without a bargain, the increase was an unlawful change in the terms and conditions of employment .72 MESSA denied the charges and argued that the St. Clair ISD waived its right to object to benefit increases by signing the Employer Participation Agreement and by acquiescing in previous years to MESSA's habit of making mid-term changes in benefits without the school district's consent.
The administrative law judge determined that MESSA was authorized to modify benefits during the contract term.73 Upon further review, an appeals commission overruled the trial court and found that MESSA and the MEA violated Section 10(3) of the Public Employment Relations Act, which states that a public labor union may not refuse to bargain in good faith. The new decision ordered MESSA to "Cease and desist in making unilateral changes in the working conditions of employees of the St. Clair Intermediate School District... without prior notification and affording time for collective bargaining with the St. Clair Intermediate School District."74 MESSA is now contesting this decision with the Michigan Court of Appeals, although a ruling may not come for several months.
The St. Clair case illustrates a fundamental point about MESSA: If the payments received from customer school districts were adequate enough to permit MESSA to increase benefits, then the payments received from school districts were also adequate enough to permit MESSA to decrease the total cost of its insurance plans without changing benefits. MESSA's taxpayer-funded customer school districts could have paid less while teachers could have enjoyed the same level of benefits as before.
The Michigan Association of School Boards points out that most private sector employers own their insurance policies, allowing for greater control over costs and benefit.75 With the current system, MESSA is the policy owner pursuant to its contract for underwriting services from Blue Cross. If school districts instead of MESSA owned their own insurance policies, the districts could route cost savings into other educational programs or they could rebate the savings back to taxpayers. Public school employees have nothing to fear, since school districts could not reduce benefits without going through the collective bargaining process.
MESSA offers six health insurance plans, but, according to several school districts, only four plans effectively exist. The six official MESSA health plans include: Super Med I, Super Care I, Super Med II, Super Care II, MESSA 250/20, and MESSA Limited. Many school districts are angry, however, because the two least expensive plans MESSA 250/20 and MESSA Limited-have restrictions on their purchase. Many school districts contend that MESSA is not providing them with a complete set of options when they consider which MESSA health plan to purchase.
The 250/20 and Limited plans are geared towards a pre-defined segment of the school district market. Specifically, those plans exist for both poorer school districts and groups of employees, such as hourly workers, who typically are paid lower wages. The MESSA 250/20 plan, for example, offers a $250 deductible with a $20 co-payment for certain procedures and protects against major catastrophe. It was developed primarily for lower-level support personnel whose monthly insurance premiums often exceed their monthly wages. Certain school districts must understand that the 250/20 and Limited plans offer minimal benefits and are targeted at a certain market segment. It would therefore be somewhat unrealistic to expect that all of a district's employees would even consider this coverage.
Even then, school districts have claimed that both of these plans are available only for certain periods of time, and these availability periods rarely coincide with contract negotiation periods when the actual health insurance plan is decided.76 Furthermore, only one school district in the state is known to participate in the MESSA Limited Plan. The districts are justified in stating that they deserve a chance to negotiate the 250/20 and Limited plans and that MESSA should make these plans more available. Consequently, school districts are generally forced to choose between the more expensive Super Med and Super Care plans. On a related note, some districts have expressed the desire to customize their MESSA health insurance plans. Doing so would give school districts the flexibility to design benefit structures in accordance with their own needs and budgets, rather than a limited choice between four very expensive plans.
In April of 1983, an article in the National Education Association's newsletter explained that the MEA had instituted a support program for unemployed teachers which provides them with career planning workshops, notification of employment openings through a "Job Search" newsletter, and prolonged insurance coverage. The article continued:
For the first few months, the Michigan Education Special Services Association (MESSA)-MEA's affiliated insurance service-picks up the cost of the health care plan a RIF'D employee had at the time of layoff. (Costs range from $61 to $240 monthly.) Even after the free coverage period runs out, pink-slipped members still qualify for MEA's group rates.77
The NEA conveniently revealed that MESSA was providing a gift of "free" insurance coverage to unemployed members of the teachers' union, but a vital question was not answered: Who ultimately pays for MESSA's gift coverage program?
This question has provoked continued concern among school districts, as districts want to know if they are paying the insurance costs of people who do not even work for them. Fairness dictates that school districts should only be paying insurance premiums for their employees, and not their "unemployees." According to MESSA's financial statements dating back to the time the gift coverage program was instituted, the only direct insurance contributions that MESSA receives from the MEA are for employees of the MEA.78 And if MESSA "picks up the cost of the health care plan," this would indicate that MESSA, rather than the MEA, pays the costs of gift coverage for unemployed members of the union. To this extent, customer school districts which pay for the overall cost of MESSA programs are absorbing the component costs of providing gift coverage to unemployed MEA members. However, in certain cases, school districts may offer to pay insurance premiums for laid off employees when the districts negotiate layoff settlements with the union.
Based upon unemployment trends in public education, the actual costs of providing insurance benefits to unemployed MEA members is probably quite small. Once the costs are spread out, the impact felt by each of MESSA's customer school districts is too minor to have any noticeable consequence on insurance premiums. This, however, does not justify the fact that both the MEA and MESSA are taking unfair advantage of their relationships with school districts. No effect is too small when MESSA is breaching the trust of its customer school districts.
One way school districts hope to minimize costs is by having employees themselves request the quantity of insurance they need. For example, school districts would incur needless costs if a family of two somehow received full-family coverage rather than two-person coverage. This is why many school districts are bothered that MESSA requires uniform coverage for participants in the MESSA PAK program. They are worried that MESSA is generating excess costs by forcing employees with varying insurance needs to subscribe to a uniform level of coverage.
The MESSA PAK program allows school districts to purchase several forms of insurance coverage from MESSA in one convenient package. Rather than purchase dental insurance from one carrier, disability insurance from another carrier, and health insurance from yet another, MESSA can combine all of these coverages into one purchase. But with the MESSA PAK program, MESSA requires uniform coverage of an employee group subscribing to a particular insurance package. This "true group requirement" mandates that every member of an employee group be covered by the same policy, with the same premiums paid for every employee in the group. Even if some employees have no need or use for all of the coverage provided by MESSA PAK, they must subscribe to it all as part of a uniform employee group. The true group requirement makes the cost of coverage more expensive than necessary, because school districts pay premiums for some employees who may never utilize certain benefits.
Suppose, for example, that a school district negotiated a MESSA PAK plan consisting of health, vision, and dental coverage into its collective bargaining agreement. The district would have to pay a fixed amount of premium per employee for MESSA PAK, even though many employees of the district will end up with duplicate coverage. An employee may receive dental and vision coverage under the MESSA PAK plan, but that same employee may also receive similar dental and vision coverage from a spouse's insurance plan. Concurrent coverage is neither necessary nor efficient, and amounts to a waste of money.
While most insurance companies will allow a customer to design a health insurance package by choosing between specific riders, MESSA does not allow its customer school districts to do this. This type of health care option, often known as a cafeteria plan, would inevitably reduce the cost of insurance, since each district or district employee could design a benefit package in accordance with their individual needs. But since MESSA will not allow this, customer school districts must choose between some of the most expensive, confined, and comprehensive insurance plans available in the state.
Although MESSA is worthy of criticism for many of the ways in which it conducts business, not all of the criticism has been leveled with fairness. A frequent subject of criticism has been the decision by MESSA and Blue Cross to eliminate dual choice of health insurance plans. The term "dual choice" refers to situations where employees are given the opportunity to choose between two competing indemnity plans. Under regular circumstances, employees would comprise one group for underwriting purposes and would not be given more than one option for insurance. Several of Michigan's school districts have persistently objected to the elimination of dual choice, even though the decision was economically prudent on MESSA's part.
In 1989, MESSA adopted a "Dual Choice Phase-Out" plan, which eliminated the co-existence of MESSA and Blue Cross insurance plans over a five year period. Although this plan might appear to be an attempt by MESSA to dominate its market, there were valid reasons for the decision which supersede any attempts to undermine it.
The dual choice option permitted public school employees to choose between MESSA coverage and Blue Cross coverage. The obvious problem with this and similar arrangements is that the plan offering more comprehensive benefits tends to be chosen by employees with a greater need for insurance. Similarly, the plan with reduced benefits tends to be chosen by people in good health, who can take advantage of rebates for selecting the cheaper plan. For example, an employee who expects to be in good health for the coming year will choose the less-comprehensive Blue Cross plan and receive a rebate. But next year, the employee may expect to become pregnant, so she will choose the MESSA plan, since it will fully cover her medical bills. This is the problem of adverse selection- one carrier retains a disproportionate share of the risk. Instead of a single group with both high and low risks, one carrier ends up with the high risk while the other enjoys the low risk.79
The existence of dual choice was an expensive underwriting policy for MESSA. Since insurance rates are based largely on actuarial predictions, the high losses for MESSA translated into higher premium rates. Under usual circumstances, MESSA had the higher number of participants, but due to the existence of dual choice, it, also had the higher risk since it provided the better benefits.
It is possible to question Blue Cross's role in the decision, once the situation is analyzed from Blue Cross's perspective. Whether the plan name is Blue Cross or MESSA, Blue Cross is still the underwriter of both plans. As the underwriter, Blue Cross incurs the same aggregate experience factor regardless of whoever has its name on the policy. Furthermore, Blue Cross benefits from underwriting MESSA plans without having to compete with MESSA. Is it just that Blue Cross was sympathetic to MESSA's losses, or did other motivations factor into the decision? (Consider that dual choice is prohibited by Paragraph 6 of the standard Blue Cross Group Operating Agreement, but exceptions were previously made for the school employee market). To further complicate matters, school districts could not tell who made the decision to eliminate dual choice, since both Blue Cross and MESSA arrived at similar, yet independent, decisions.80 Nevertheless, the decision to eliminate dual choice was an intelligent move for MESSA, since it spread total risk and eliminated the problem of adverse selection.
The design of the MEA complex in East Lansing is an appropriate indication of the extent to which the MEA and its subsidiaries are involved, in each other's operations: all four corporate headquarters are connected by a skywalk. Perhaps an even more revealing indication occurred in March of 1993, when a MESSA receptionist greeted a phone call from the Detroit News by stating, "MEA ... er, MESSA."81 The simple fact of the matter is that the four corporations which comprise the "MEA Family," as the MEA calls it, are all interrelated in various ways. There is, of course, the underlying foundation of the interrelationship, namely that all four corporations are owned and administered by the MEA. Moreover, the operations of the four corporations are significantly integrated with one another and part of a systematic exchange of resources. Most importantly, the corporations are predominantly governed by and subordinate to the will of the MEA.
One of the first things the public must clearly understand about MESSA is that it is an extension of the MEA-devised by the MEA, owned by the MEA, and controlled by the MEA. This presents obvious concerns about the MEA's ability to influence the decisions and conduct of MESSA, because any imposition of the MEA's will over MESSA would inevitably have some effect on MESSA's interactions with its customer school districts. In the sense that the MEA is more concerned about maximizing benefits for its members and less concerned about minimizing costs for school districts, the consequence of MEA control over MESSA is most likely that school districts are shouldering a burden of excess costs because the MEA has actively sought greater benefit thresholds from MESSA. In general, the conduct of MESSA towards its customer school districts does have something to do with the MEA's involvement in MESSA, and this is having an impact on public education.
The best way to understand MESSA as an extension of the MEA is to examine the essential aspects of their relationship, which include their commercial affiliation, the degree of control maintained by the MEA, and the integration of their operations. After doing so, it is possible to reach a general conclusion about MESSA in relation to the MEA: MESSA is an agent of the MEA, and it is manipulated in the MEA's favor, with little regard for the consequences to Michigan's school districts.
The entire relationship between MESSA and the MEA is premised upon their commercial affiliation. Since MESSA is one of its wholly-owned subsidiary corporations, the MEA is often referred to as MESSA's "parent corporation." In this capacity, the MEA maintains "fiduciary" control over MESSA, meaning that it governs MESSA through a position of trust. For example, MESSA is managed by its own executive director, but this person is hired and supervised by the MEA. Even though MESSA's corporate registration papers reserve such powers to the MEA, the MEA is not restricted by this distribution of authority. As a parent corporation, the MEA has a legal right to exercise absolute control over MESSA.
When considering a relationship similar to the one involving MESSA and the MEA, the United States Supreme Court offered a relevant interpretation of how these parent subsidiary enterprises function:
A parent and its wholly owned subsidiary have a complete unity of interest. Their objectives are common, not disparate; their general corporate actions are guided or determined not by two separate corporate consciousnesses, but one. They are not unlike a multiple team of horses drawing a vehicle under the control of a single driver. With or without a formal 'agreement,' the subsidiary acts for the benefit of the parent, its sole shareholder... They share a common purpose whether or not the parent keeps a tight rein over the subsidiary; the parent may assert full control at any moment if the subsidiary fails to act in the parent's best interests.82
In the case of MESSA and the MEA, both corporations are directed by the will of the MEA for the common purpose of providing benefits and services to the MEA's members.
The reason why the MEA created an insurance subsidiary is best described in MESSA's original Articles of Incorporation. The mission statement of MESSA was explained, in part, as follows:
This Association is organized for the purpose of carrying on business as an insurance agent, including the administering, servicing, and promotion of insurance and working out programs relating thereto of all types and kinds for the benefit of the members of the Michigan Education Association...83
This statement concisely refers to MESSA as an "agent"-an interesting concept in itself if the MEA is the principal-and identifies MESSA's objective as developing insurance benefit programs to the advantage of MEA members. In 1980, MESSA redefined itself as a "voluntary employees' benefits association" (VEBA) and deleted any reference to agency. In order to qualify as a VEBA, MESSA must provide benefits to its members, who must be affiliated through a work-related bond, in this case, the MEA. Nevertheless, the corporate conscience guiding the actions of both organizations belongs to the MEA; hence, MESSA is ostensibly acting on behalf of the MEA. To distinguish between an insurance agent of the MEA and a voluntary employees' benefits association of the MEA is not to suggest that MESSA no longer acts as an agent of the MEA.
The concept of limitations on who can take advantage of MESSA benefits is also essential to MESSA's commercial affiliation with the MEA, because MESSA's membership base is a product of the MEA. In order to receive MESSA benefits, public school employees must be employees of the MEA and its subsidiaries, members of MEA-affiliated bargaining units, administrators employed by MEA-affiliated school districts, or eligible retirees of the public education sector.84 In simplest terms, the MEA must be an active force in a school district before any of the district's employees can be eligible for MESSA coverage
Perhaps the best way to characterize MESSA's commercial affiliation to the MEA is to speak in terms of "dependence." After all, MESSA is dependent on the MEA for its very corporate existence, in addition to the mission and membership base provided through affiliation with the MEA. Along similar lines, MESSA is also dependent on the MEA for authority and governance. The MEA has managed to keep tight reins on MESSA by imposing control on MESSA's operations.
If there was any doubt that MESSA and the MEA have a single corporate conscience, an analysis of MESSA's decision-making cabinet should eliminate all skepticism. As stated in an MEA pamphlet, "MESSA is a part of the MEA Family. It's a membership organization governed by MEA members."85 The members of the "MEA Family" and their interlocking governing structure is shown in Figure 2. The MEA maintains control over MESSA through the authority of the MEA executive director and MESSA's thirteen member Board of Trustees. All of the decisions relating to the official business policies and practices of MESSA originate within this Board. With its leverage on the MESSA Board, the MEA is able to implant its will into MESSA's operations.
The two most recent appointees to the MESSA Board of Trustees are the incumbent president and vice president of the MEA.86 In addition, six of the trustees are elected from and by the MEA Board of Directors. The five remaining trustees are elected from the MESSA membership by MESSA's voting members, which include incumbent MESSA trustees and officers along with all MEA directors who are also MESSA members. Therefore, the MEA still has a prominent role in electing the five other trustees.
All trustees are appointed to three year terms, but the eight trustees sponsored by the MEA may only hold appointments while incumbent in their MEA positions. In short, eight of the thirteen people who actually control MESSA also control the MEA. The five remaining officers are selected in part by other people who control the MEA. According to the definition of a quorum in MESSA's bylaws, the MEA members alone constitute enough members to conduct valid transactions of business.87
Every year, the MESSA Board of Trustees must also select its executive officers. As outlined in the bylaws, "The Board shall select as Secretary and Chief Executive Officer of MESSA the Executive Director of MEA, whose title shall be Executive Secretary of MESSA."88 The executive director of the MEA follows suit by appointing the executive director of MESSA, who serves as its chief administrative officer. In addition to the role of executive secretary, the MEA's executive director serves as corporate treasurer of MESSA.89 In other words, the person who controls the MEA is ultimately responsible for MESSA's money. Recently, Beverly Wolkow of the MEA conceded the point by acknowledging that she fulfills two roles as the "Chief Executive Officer" of both MESSA and the MEA.90
MESSA is particularly sensitive about accusations that it is controlled by the MEA. The standard rebuttal contends that all MESSA trustees are conditioned to eliminate any bias towards the MEA which might impair their fiduciary obligations to MESSA. The trustees do, in fact, participate in an annual training seminar, which explains their position of trust for MESSA. According to MESSA's attorney, "The training is intended to insure (sic) that those trustees who have dual roles, as well as the independent trustees, understand that while sitting on MESSA's board, the decisions they make must be in MESSA's best interest."91 But does this training absolve MESSA of control by the MEA? The judge in the latest court case involving MESSA did not think so, when he stated: "Although the testimony describes various conflicts between the MEA and MESSA, and the MESSA Board members receive 'training' regarding their fiduciary duty to MESSA, the evidence of independence or separation from the MEA Board is insufficient to overcome the evidence of control and agency."92 As previously mentioned, even if the MESSA Board of Trustees did not consist predominantly of MEA directors, the corporate affiliation of the two companies still permits the MEA to exercise control over MESSA.
MESSA cannot establish its independence from the MEA because of the MEA's ownership and control; therefore, the decisions of MESSA almost always appear to reflect the larger concerns of the MEA. For example, one document identifying MESSA's mission for 1988-90 illustrates MESSA's subservience to the MEA:
MESSA's mission is to serve the members of the Michigan Education Association by providing comprehensive health and related employee benefit plans which respond to the financial and special requirements of the membership with a continued commitment to personalized service.93
The document goes on to explain the "goals, objectives, and strategies" of MESSA, which clearly coincide with those of the MEA. Included among these are the following:
"Participate in the development of a coordinated membership system that will meet the needs of the MEA and the constituent organizations and programs."
"Strengthen the working relationship between MESSA and the MEA to enhance service delivery to the membership."
"Facilitate the greater input of the MEA, MEDNA, and MEA Financial Services leadership in the critical decisions and activities of MESSA through improved communication and consultation."
It seems as if the MEA has dictated the crucial priorities and policies of MESSA. This is not to suggest, however, that MESSA cannot think for itself. The Executive Director of MESSA is given reasonable latitude in deciding matters which relate strictly to the business of administering insurance and managing the organization. Yet, when the issue at stake involves even a remote interest of the MEA, the MEA will often signify its intentions. If MESSA ever did make a decision in disregard of the MEA's desires, the MEA would almost certainly intervene.
With its domination of the MESSA Board of Trustees, the MEA obviously exercises a considerable degree of control over MESSA. How does this affect Michigan's school districts? The most important power retained by the MEA pertains to the actual construction of MESSA insurance coverage. School districts need to realize that the MEA ultimately approves MESSA's insurance plans, and once a school district signs a contract for MESSA coverage, it surrenders exclusive authority to the teachers' union regarding:
Control of premium prices. The MEA authorizes the annual premiums which school districts pay in order to receive employee insurance. If a limit to annual premium increases has been negotiated, employees may need to participate in the premium increase, but school districts tend to absorb the rising costs.
Design of benefit packages. The MEA approves the design of the benefit packages and has the discretion to change the level of benefits at any time without consulting MESSA's customer school districts. This authority is now being challenged by the St. Clair Intermediate School District in a court of law.
Payment of claims. MESSA's claims processing system is operated by various employees of the MEA conglomerate. Claims are paid in such a way that the interests of the MEA members are given priority above the interests of school districts or taxpayers.
Size of reimbursements. Under normal circumstances, the "reasonable and customary" fee schedules which determine the reimbursements for covered services would be determined by MESSA's underwriters. In the case of MESSA's health plans, however, the MEA endorses the fees that are paid to providers who do not participate with Blue Cross/Blue Shield of Michigan. The MEA reduces the personal liability of its members by setting a fee schedule well above the Blue Cross schedule. This schedule, which may be set 15 percent higher than the similar Blue Cross schedule, contributes to the rising cost of health care, and only the MEA can change it.
Expenses for administration. School districts can hold the MEA accountable for MESSA's high administrative expenses, because the MEA both supervises the expenses of MESSA and can alter these expenses at any time in various ways. One way the MEA could decrease expenses is by adjusting the efficiency of MESSA's claims processing department. Several years ago, for example, the MEA hired summer interns from nearby Michigan State University, but when the interns outperformed regular MESSA employees and depleted the work supply, the program was discontinued.
By all indication, the MEA will not relinquish its aggressive control over MESSA at any future point. Judging from the integration of both corporations, it is apparent that MESSA could not survive without rigid control by the MEA, and the MEA would suffer a curtailment of power if it could no longer manipulate MESSA. Of course, MESSA's unique benefit packages allow the MEA to guarantee that members will be loyal. If this enforcement mechanism were eliminated, the MEA might falter, but eventually regain strength. In the opposite case, MESSA could not function if it ever stopped collaborating with the MEA.
| Figure 2: MEA-Subsidiary Interlocking Boards | ||||||
| Executive Members | MEA | MESSA | MEDNA | MEA Financial | Verity Insurance | MEA Legal Services |
| Beverly Wolkow | Executive Director | Executive Secretary | Chairperson | Chairperson | Executive Secretary; Incorporator | |
| Julius Maddox | President; Board Member | Board Member | President | Board Member | Board Member | |
| Steve Cook | Board Member; Secretary/ Treasurer | Board Member | Board Member; Secretary/ Treasurer | Board Member | ||
| Herb Surtman | Executive Director | Controller/ Treasurer; Incorporator | ||||
| Warren Culver | Executive Director; Board Member | Incorporator | President | |||
| Trini Johannesen | Vice-President; Board Member | Board Member | Board Member | |||
| Bill Williams | Board Member | Vice- President; Board Member | ||||
| Peggy Watkins | Board Member | Chairperson; Board Member | ||||
| Patrick Furner | Board Member | President | Incorporator | |||
| Guy Sands | Board Member (NEA Representative) | Board Member/ Treasurer | ||||
back to The MEA's Control Over MESSA
The final step of the analysis of MESSA's relationship with the MEA is to consider how these corporations actually interact. In combining their commercial affiliation with the MEA's control, the business activities of both MESSA and the MEA are deeply enmeshed. According to one annual report of the MEA with a separate section on MESSA:
Since September 9, 1960, the date on which the Michigan Education Special Services Association was chartered as a Michigan non-profit corporation, we at MESSA have maintained a very close affiliation with the MEA through the latter's sponsorship of MESSA programs.94
The bulk of these interactions concentrate on an exchange of labor resources and a cooperative marketing strategy for promoting MESSA insurance to MEA members.
Given the presence of MESSA employees on the MEA's bargaining teams during contract negotiations and private caucus meetings, there is an obvious exchange of labor resources taking place between MESSA and the MEA. The same MESSA employees who participate on bargaining teams also use the MEA's offices, regional facilities, equipment, and secretarial personnel.95 Furthermore, MEA employees have been known to act as operatives for MESSA. As noted in a report compiled by the law firm of Mosher, Vondale, Gierak & Baumhart:
The fact that MESSA pays the MEA millions of dollars for services is documented. What such documents do not show are the large numbers of employees who are paid by both MESSA and the MEA, even though they spend the vast majority of their time doing strictly MEA work. Even full-time MESSA employees do a significant amount of work on behalf of the MEA.96
This employee interchange could be anticipated, considering that the majority of employees in the "MEA Family" are represented by the same union (United Staff Organization), form homogeneous collective bargaining units and, are covered by the same collective bargaining agreement.
The prime motive for this exchange of labor resources is to facilitate the marketing of MESSA insurance plans. In 1981, MESSA and the MEA took advantage of their relationship and developed a cooperative marketing strategy for promoting MESSA insurance. Since MESSA's programs are restricted to public school employees with some connection to the MEA, the most sensible approach to marketing MESSA's products is for MESSA to take advantage of the MEA's influence among its membership. The MEA already has the means to communicate with its members, so rather than have MESSA cultivate its own similar lines of communication, the MEA has assumed the responsibility for promoting MESSA to its membership.
In short, the MEA "markets" MESSA by puffing its programs to MEA local affiliates and encouraging the units to incorporate MESSA into their collective bargaining agreements. The MEA dispatches its Uniserv division of professional contract negotiators into school districts at the time of contract negotiations. Using conventional sales tactics, the Uniserv negotiators sing the praises of MESSA and encourage the MEA local affiliates to demand MESSA from their districts, resorting to strike threats as necessary. The objective is to rally the local teachers' union around MESSA and force the district to acquiesce to this demand. If the union and the school district agree to a MESSA insurance plan, the Uniserv negotiators use a booklet of "prototype contract language" to incorporate MESSA into the contract.
The MEA will not admit that it wants to force every school district to purchase MESSA coverage. However, in 1989, the MEA delineated a five year plan to "negotiate MESSA as the exclusive health care benefit plan in all collective bargaining agreements" beginning in the 1991-92 school year.97 The attorneys for MESSA reminded their critics, "Although it is the official MEA policy to try to bargain MESSA benefits for the MEA members, many MEA bargaining units do not have MESSA plans written into their collective bargaining agreements."98 Nonetheless, they concede that the MEA does have an official policy mandating that the Uniserv division attempt to negotiate MESSA coverage whenever possible.
Related to the MEA's efforts at marketing MESSA programs is the MEA's efforts at promoting the quality of MESSA coverage to those who already have it. This type of member retention program has been developed to ensure that the MEA members who have MESSA coverage appreciate the program and understand that the MEA makes the benefits possible. The interest of the MEA is obvious: effective inter-union marketing will foster confidence in MESSA, which assures the MEA that members will remain loyal to MESSA and the union. The essence of these promotional devices is captured in the advertisements and publications which the MEA produces for member consumption. For example, a promotional flyer distributed by the MEA in 1989 persuades teachers: "Your health insurance is an important part of your compensation package. It should not be under the control of anyone but you and your organization: the MEA."99
The leadership of the MEA habitually promotes the virtues of MESSA insurance to members of the union. By every indication from the amount of persuasion involved, it would be quite difficult to convince teachers that other insurance plans deserve any attention. Even if school districts could find similar coverage at a more affordable cost, the odds of persuading the teachers to abandon MESSA are against them.
The debate over whether or not MESSA is an "agent" of the MEA merits special attention. Because it is a public employee union, the Michigan Education Association is supposedly regulated by the Public Employment Relations Act (PERA) of 1947, although it has little regard for this Act.100 PERA was designed to govern the conduct of public sector labor unions in regards to strikes, workers' rights, bargaining duties, and contract negotiations. The practice of a public employee union establishing subsidiary corporations was not explicitly addressed in PERA or related legislation. As a result, a complicated legal question has arisen as to whether or not a union's subsidiaries are also regulated by PERA. This question is now being considered in the case of IEA/MEA and MESSA v. St. Clair Intermediate School District, which is pending before the Michigan Court of Appeals. Specifically, the issue at stake is whether MESSA is an agent of the MEA and therefore subject to the same regulations as the MEA.
Before any unfair labor practice charge can be brought against MESSA, the law must ascertain that MESSA is the agent of a labor organization-the MEA. Otherwise, MESSA is not subject to the jurisdiction of PERA. Due to the significant marketing role that MESSA has in the collective bargaining process, it was inevitable that an unfair labor practice charge would arise, as demonstrated in the aforementioned case. In that particular case, MESSA unilaterally increased the lifetime maximum benefit of its insurance plans without consulting its customer school districts. Under the changed system, MESSA members could receive up to $2 million in lifetime benefits rather than the previous $1 million limit.
The St. Clair Intermediate School District contends that MESSA has an obligation to negotiate such changes with school districts, because MESSA is the agent of a labor union. MESSA, on the other hand, contends that while it is owned by the MEA, it conducts business independently of the MEA. Based upon the "synonymy" between the organizations, the symbiotic relationship between the officers, and the degree of control exercised by the MEA, the administrative law judge established that MESSA is an agent of the MEA, subject to control by the MEA.101 The first appeal of the case affirmed this finding of fact.
The law of agency is based upon common law principles of control. Before the Court of Appeals can rule that MESSA is an agent of the MEA, it must determine that the MEA has the ability to control MESSA, that MESSA has the authority to act for the MEA, and that there is a definitive relationship between these organizations.102 In requesting the appeal, MESSA argued that "corporate control does not mean that the controlled entity acts as an agent of the parent entity for all purposes."103
The forthcoming decision from the Court of Appeals will set a precedent for future judgments relating to MESSA. If the decision is upheld that MESSA is an agent of the MEA, it will clear the way for current and future unfair labor practice charges which are brought against MESSA. However, if this decision is reversed, the consequences would be devastating to public school districts which contend that MESSA has violated their rights as parties to an agreement. MESSA would be given the means to alter its insurance agreements without the consent of school districts, since it will have no duty to bargain with school districts once a labor contract has been signed. If MESSA loses the case, however, it would mean that the MEA is legally liable for the actions of MESSA, which contradicts one purpose of having corporate subsidiaries-to spread risk and limit the liability of the parent corporation. Either way, the results will be a serious blow to the losing party.
One of the unavoidable problems of taxation is that citizens may subsidize causes with their tax dollars which, given a choice, they would otherwise not support. For example, many taxpayers would not contribute to the Michigan Education Association if given this option, but they end up supporting the union since a portion of their tax bill is applied to the MEA through educational spending. In a less obvious way, taxpayers also support the MEA whenever a school district purchases employee insurance from MESSA, because a portion of MESSA's income is channeled into the MEA and its related divisions. In 1992, for example, after MESSA paid for benefit costs, 35.4 percent of its remaining revenues were paid to the MEA and the Michigan Education Data Network Association in the form of "service fees."104
In effect, the MEA is receiving an annual "commission" for representing MESSA in contract negotiations with school districts. The commission (or service fee) supposedly encompasses all of the costs incurred by the MEA while bargaining on behalf of MESSA, marketing MESSA programs to its members, and representing MESSA's interests in the political arena. Yet, the bulk of MESSA's service fees-84 percent in 1992 are paid to MEDNA in exchange for various clerical services. Astute observers have questioned this whole financial exchange, noting that while MESSA and the MEA cannot accumulate profits, MEDNA has "for-profit" corporate status.
The practice of purchasing services from related corporations is not unusual. In fact, it is a legitimate way to transfer funds between corporations so that one has more available cash. With MESSA, the MEA is given an additional source of income independent of member contributions. MEDNA, on the other hand, makes it possible for the MEA to access a powerful computer system and other shared resources that would be nonexistent but for MESSA. MESSA owns a massive network of computers, MEDNA operates the system, and the MEA is given access to the computing resources as well as the information contained within MESSA's database. Rather than purchase its own comparable resources or lease them directly from MESSA, the MEA has pooled interests with MEDNA.
There are numerous questions which need to be answered with regard to the MEA financial network. How are these transactions affecting public education? What does it mean to taxpayers besides indirect financial support of the teachers' union? For what purposes are the MEA and MEDNA using the money they receive from MESSA? The answers can be found in the actual transactions between the MEA, MESSA, MEDNA and MEA Financial Services.
In 1981, the Executive Directors of MESSA and the MEA entered into a compact which has since served as the basis of the financial relationship between the two corporations.106 Entitled the "Marketing and Service Program Agreement," the document lists the vague guidelines of a complete financial exchange in just over three pages. As explained in the agreement, MESSA will compensate the MEA for various marketing, legislative, and research expenses, along with a rental fee for "various offices around the state." In return, the MEA will "utilize its personnel" in order to enhance enrollment in MESSA programs and improve service to MESSA participants.
The agreement is a joint venture, where MESSA primarily benefits from having access to the MEA's resources and representation during contract negotiations. In turn, the MEA gains favor with its membership by "sponsoring" MESSA's innovative but costly insurance benefits. The objectives of the agreement are stated towards the beginning of the document: 107
"All MEA local units will participate in MESSA programs."
"All MEA local units will seek maximum benefits under MESSA programs."
"All MESSA members will receive the best and most responsive service attainable, which will be better than that available from any other administrator or insurer."
There is already cause for concern at this point, because the objectives demonstrate that the desired end of this financial exchange is to have MESSA dominate the market for provision of insurance to public school employees. The consequence to public education, of course, is that school districts are forced to shop in a market with little or no competitive pricing. And with each subsequent section of the agreement, the problems compound:
Representation in contract negotiations. The MEA maintains a staff of professional contract negotiators known as the Uniserv division. Pursuant to the agreement, Uniserv develops strategies that make every reasonable attempt to incorporate MESSA insurance into labor contracts with school districts. In cases where the goal of maximum participation in MESSA programs has not been attained, "appropriate corrective action" is taken.108 Since the Uniserv division is managed and paid by the MEA, MESSA must reimburse the MEA for representation during contract negotiations. But what the transaction effectively amounts to is a gratuity for MESSA's unfair bargaining advantage of having contract negotiators on its side. This practice raises further questions about damage to competition, since no other insurance administrator can contract for representation with the group that bargains for most public school employees.
Lobbying and political activity. MESSA also uses funds received from school districts for unspecified political purposes, in conjunction with the MEA. The one-sentence section subtitled "Public Affairs" states:
With respect to legislation which has an impact on MESSA programs, MEA and MESSA will coordinate their efforts in legislation deemed beneficial to MESSA. 109
An addendum to the agreement added that MESSA now reimburses the MEA for the cost of a full-time lobbyist in the MEA's Government Affairs Division, even though MESSA employees also devote time to similar activities."110
No criteria is identified for determining the legislation which might impact MESSA, and any such criteria is assumed to be purely subjective. According to a MESSA promotional flyer from April of 1989, "MESSA and MEA work together to represent MEA members when dealing with your legislative needs on the state and federal levels."111 Yet, for all the public knows, the "legislative needs" of MESSA members could be private endorsements of political candidates or battles against legislation which would permit school districts to locate the most cost-effective insurance administrator-all conducted with money that was intended to provide public school employees with insurance benefits.
The MEA division which actually contributes to political causes is the Michigan Education Association Political Action Committee. The MEA PAC contributed $1,461,442 to its political allies in 1992 alone-with the majority given to the Democratic party and its assorted constituencies, such as the Fund for a Democratic House, the House Democratic Campaign Committee, and the House Democratic Victory Fund.
The use of public funds collected from school districts for political purposes is an abuse of taxpayer trust, because those funds were given a specific, non-partisan intent. The necessity of these lobbying expenditures is further cause for concern because it is likely that MESSA is using the money to oppose legislation which might improve matters for public education at the expense of MESSA.
Other stipulations. MESSA also pays the MEA for various research, information, and consultation services. The MEA collects information for MESSA pertaining to budgets, labor contracts, and fringe benefit levels in school districts. Included in the overall service fee is the cost of an employee in the MEA's Professional Development/Human Resources department.112
Calculating the service fee. Another deficiency of the operating agreement between MESSA and the MEA is the lack of specificity for determining which expenses MESSA will cover. The service fee is based on items such as information that may have an "impact" on MESSA programs or "legislation deemed beneficial to MESSA," but the agreement fails to explain how impact or benefit will be measured.113 If the parties have made no reasonable attempt to identify the goods, how can the transaction be completed? How is MESSA figuring the precise amount of funds that it will transfer to the MEA? The document merely suggests that on September I of every year, before MESSA even takes advantage of MEA services, the parties determine the "fair market value" of the services MESSA is supposed to use during the upcoming year. Any specific expenses are added to the estimated cost of utilization, and disputes can be adjudicated by an auditor. Yet, this "calculation" would appear somewhat deceptive if there is any truth to the testimony of a former MESSA trustee, who noted in conversation that MESSA is not provided with any details or line item cost breakdowns of the annual service fee.
The Funneled Funds. Between 1981 and 1992, the MEA received approximately $12 million in direct payments from MESSA-money that MESSA received through taxpayer support of education. This figure excludes the annual rental payments MESSA has made to the MEA since it began leasing MEA property in 1974.114 The service fees for the past 10 reporting periods are shown in Table 1.
Even though the service fee increased 61.5 percent over this 10 year period, the annual increases have generally kept pace with the rate of inflation. Based upon the trends revealed in the yearly updates to the operating agreement, roughly 16 percent of each annual fee can be applied to legislative and research services with the remaining 84 percent applied to marketing services rendered by the MEA's Uniserv division.
| Table 1 | |
| Payments for Services Made to the MEA by MESSA |
|
| 1983 1984 1985 1986 1987 1988 1989 1990 1991 1992 |
$953,000 $993,000 $1,034,000 $1,065,000 $1,055,000 $735,000* $1,235,000 $1,329,000 $1,434,000 $1,549,000 |
*Effective June 30, 1988, MESSA changed its fiscal year from November 30 to June 30, in order to coincide with insurance company contracts. The 1988 dollar figure represents a seven-month period, rather than a complete fiscal year.
Of all the directions in which MESSA routes funds, the most ambiguous involves MEDNA. One year after MESSA and the MEA entered into their operating agreement, MEDNA was incorporated for the purpose of providing administrative and clerical services to the MEA and its subsidiaries.115 MEDNA is physically located between the offices of the MEA and MESSA, and is essentially subject to the MEA's control. (The President of the MEA is President of MEDNA and the Executive Director of the MEA is the Chairman of the MEDNA Board.)
Both the MEA and MESSA contract with MEDNA for data processing equipment, computer time, accounting services, billings services, financial report preparations, and so on-services that could otherwise be maintained independently. At first glance, it is not readily apparent why the MEA and MESSA must contract with a separate firm to provide their clerical services; nevertheless, they pay out millions of dollars every year to MEDNA for these services. Furthermore, MESSA's financial statements reveal that MESSA guarantees various loans for MEDNA and leases equipment to MEDNA.116 If each corporation is separately purchasing resources for MEDNA, such as computers, and then contracting with MEDNA for access to all of its resources, then the MEA and its subsidiaries are pooling resources for the whole conglomerate. The MEA is 'providing an economy of scale by centralizing a common operation and reaping the benefits of having MESSA subsidize the operations of its related corporations by giving them access through MEDNA to MESSA-purchased resources.
MESSA provides MEDNA with approximately 60 percent of its income, so without MESSA's financial support, MEDNA probably could not afford to stay in business.117 If MESSA did not provide so much operating revenue to MEDNA, it is obvious that the whole MEA conglomerate would suffer the impact of reduced access to resources through MEDNA.
According to MESSA's financial statements, its payments to MEDNA are based upon utilization of telephone services, labor relations, financial services, buildings and grounds maintenance, staff training, and development of all required data processing and computer services. The amounts paid to MEDNA for the past 10 reporting periods are shown in Table 2.
Is it necessary for MESSA to purchase certain services from MEDNA that it otherwise could not obtain, or is MESSA using the money that it collects from school districts to help enrich the computer and other resources of the whole MEA conglomerate? The answer is not simple to discern, because the MEA is very protective of information about MEDNA's operations. But if the latter is true, and evidence does suggest that it is true, then MESSA has some explaining to do.
| Table 2 | |
| Payments for Services Made to the MEDNA by MESSA |
|
| 1983 1984 1985 1986 1987 1988 1989 1990 1991 1992 |
$1,278,400 $1,558,002* $2,339,300 $3,522,000 $4,985,000 $1,306,000 $5,356,000 $6,139,000 $6,834,000 $8,285,000 |
*On September 1, 1984, MESSA entered into an agreement with MEDNA for certain administrative services. After this date, MESSA paid MEDNA a lump sum for services rendered by MEDNA. The figure for 1984 includes separate payments in the amounts of $1,455,264 for data processing and $102,738 for administrative services.
MEA Financial Services may have been created in order to compensate for the insurance programs which MESSA could not legally provide, but that does not mean MESSA has no interest in MEA Financial Services. In 1992, MESSA advanced $3 million to MEA Financial Services in order to capitalize the Verity Insurance Company, a wholly-owned for-profit domestic insurer. Verity underwrites long term care insurance programs, which the MEA can negotiate as an additional benefit in labor contracts. According to the Michigan Insurance Bureau's latest statistical report, the Verity Insurance Company is located at the same address as both MEA Financial Services and MEDNA. In 1991, it did not write any direct premiums, but finished the year with a $2.8 million net worth.
Since MESSA advanced $3 million to MEA Financial Services in order to purchase Verity, MESSA, as the financier, has a financial claim to Verity. Final maturity is not scheduled to take place until September 1, 2002. In effect, MESSA has purchased an insurance company which is managed by another MEA subsidiary. School districts across the state should be alarmed by this. With Verity in place and the MEA on its side, school districts could end up with larger bills for employee insurance if MEA local units begin demanding Verity benefits in addition to MESSA benefits. Nevertheless, there is one question every school district should pose to MESSA: Why is MESSA funding the multi-million dollar purchase of an insurance company when it could be reducing premiums for its customer school districts?
With all of the problems that MESSA has created for public education in the state of Michigan, it is quite evident that the state must scrutinize the MESSA operation and consider corrective measures to alleviate its overall waste and inefficiency. With public awareness and outrage about MESSA surmounting, the time has come for a thoughtful debate over MESSA. In late September of 1993, the Michigan Insurance Bureau announced that it is initiating a discussion of MESSA; the Bureau is performing a routine market conduct exam of MESSA in response to several complaints from the public. An article in the Detroit News on September 22, 1993 stated:
The probe began after allegations that MESSA adds unnecessary costs to taxpayer-supported school employee health insurance and it is funneling profits to the Michigan Education Association to use for the union's political lobbying and other purposes...118
Warren Culver, the executive director of MESSA, denied any wrongdoing by stating, "It sounds to me like [the deputy insurance commissioner] is shooting in the dark." The facts will speak for themselves. Yet, assuming the state does determine that a legislative response is necessary to combat the deficiencies of MESSA, is there any likelihood that corrective measures will ever be enacted? The chances are slim that MESSA will ever be forced to comply with any regulations or standards of operating efficiency, unless a major impediment can be avoided. That impediment to reform is the MEA's ability to sway public policy in its own favor otherwise known as the MEA political machine.
The MEA political machine is essentially composed of two parts: the MEA's office of government affairs and the MEA Political Action Committee. In addition, the MEA is able to involve its membership and staff in massive grass-roots political campaigns whenever issues arise which concern the MEA's interests. The MEA is well known for unleashing its political muscle every time a major public policy initiative appears which might impact the union or affect its political interests. In the spring of 1993, for example, the MEA was one of the more fervent supporters of the sales tax increase contained in the failed Proposal A ballot question. In previous years, the MEA has led similar statewide efforts to increase Michigan's sales tax. The MEA has also championed causes not directly related to educational concerns, such as the movement to sustain Medicaid-funded abortions. In fact, Right to Life of Michigan claims that the MEA is one of the leading pro-choice advocacy groups in the state.
The MEA political machine is so effective at what it does because it boasts huge amounts of financial contributions from MEA members as well as an influential lobbying staff. The MEA's lobbying division continually targets issues relevant to the union, determines an appropriate stand, and then coordinates a strategy for action. As a whole, the MEA is quite vocal in expressing its political desires to Michigan's legislators, and it is not afraid of applying pressure tactics whenever it seeks responsive action from the legislature. For now, the MEA's political persuasion and potency of influence is unmatched by any other public employee union in the state, which is why MESSA's critics are fearful.
The immediate concern coming from school districts and other MESSA critics is that any proposed action with even the slightest chance of hurting MESSA's operations would be struck down by the MEA political machine. Any legislative measures calling for tighter regulations of MESSA, compelling MESSA to operate more efficiently, opening up MESSA's market to competitive bidding, etc., would encounter certain opposition from the MEA. The MEA's motives are clear, given that MESSA provides the MEA with significant resources and membership strength.
Through past lobbying activities, the MEA has proven that it has the means to wage a war against any anti-MESSA/pro-school district efforts. In 1991, for example, Senator John Pridnia of Hubbard Lake and Representative Beverly Bodem of Alpena introduced bills in the Michigan legislature which would have mandated competitive bidding of health insurance in school districts. According to the Michigan Association of School Boards, the MEA rallied its members, and legislators each received hundreds of letters of opposition to these bills.119 Any similar legislation will most certainly encounter the same response. MESSA's critics are worried that with the MEA's vested interest in MESSA, it will be more adamant than usual about protecting its insurance subsidiary.
To complicate matters, many legislators are not willing to take a stand against the MEA because of imminent political repercussions from the union. Consider that very few public officials even bother to enforce laws which make it illegal for public school teachers to strike in the state of Michigan. In 1992 alone, the Michigan Education Association Political Action Committee contributed funds to 78 state representatives, 18 state senators, and one justice of the Michigan Supreme Court.120 (See Appendix 1). This excludes contributions by numerous other political action committees that were funded through donations from the MEA PAC. Many school districts have expressed their objections about MESSA to their representatives in Lansing, but few lawmakers have made any demonstrable response. Officials at all levels of the state government are aware that MESSA is a cause for concern, yet there has still not been a concerted effort in the past to address publicly the problems of MESSA.
Some legislators, such as Representative David Jaye of Shelby Township, have introduced legislation in recent months that would mandate competitive bidding of insurance in all public school districts. (The MEA successfully fought off this bill.) Other public officials, such as Governor John Engler and Senator Jack Welborn of Kalamazoo, have openly acknowledged their reservations about MESSA.121 Still others have consistently evaded the issue, such as Attorney General Frank Kelley.122 Consequently, many school districts are wondering if they have been betrayed by lawmakers who fail to protect the interests of public education.
Along similar lines, many school districts are wondering if the Michigan Insurance Bureau is capable of conducting an objective investigation of MESSA. These concerns stem from Governor James Blanchard's appointment of Herman Coleman to the office of Insurance Commissioner in 1985. Herman Coleman served as Executive Director and Secretary of the Michigan Education Association from 1973 until 1980. While working for the MEA, he was a recognized expert on striking. He co-authored the Michigan "secret master blueprint" for strike action in 1973, which led to more than 50 illegal teacher strikes in that year alone.123 In the early 1980s, he was sent to Mississippi to run the statewide teachers' strike for monopoly bargaining. During his affiliation with the MEA, Mr. Coleman was treasurer of the MEA Political Action Committee.124 Evidence also suggests that he was either an employee or a paid consultant of the MEA and/or the NEA at some point after 1980.125 And throughout his tenure with the MEA, Mr. Coleman served as Chief Executive Officer of MESSA.
Numerous questions have arisen as to whether Commissioner Coleman's appointment constituted special treatment for MESSA. In his capacity as Insurance Commissioner, Herman Coleman oversaw all requests for investigations of alleged insurance fraud, including a petition filed in 1985 by 15 school districts which requested that the Insurance Bureau investigate possible violations of the Insurance Code by MESSA. The seeming conflict of interest between an Insurance Commissioner with ties to MESSA and an Insurance Bureau which oversees MESSA soon became apparent.
In a letter dated October 4, 1985, two days after his appointment, the attorneys for the 15 school districts asked Commissioner Coleman to disqualify himself from the proceedings. The letter stated:
We, therefore, believe that your prior employment and/or relationship with [MESSA and the MEA] will engender sufficient personal bias and partiality such that a fair and impartial proceeding in this case will be unavailable to [our clients], and that your disqualification is, therefore, warranted.126
In his reply, Commissioner Coleman denied the request for self-disqualification, while offering a commitment to fairness and impartiality.127 finally did deny the school districts' request for a contested case hearing-three years after the initial request was made. According to the attorneys for various Michigan school districts, it was not uncommon to experience such "inordinate delays" when asking Commissioner Coleman to investigate MESSA.128re is no reason to suspect that the current Insurance Commissioner, David Dykhouse, will have any bias either for or against MESSA; nevertheless, the memory of Herman Coleman lingers on and many school districts are still concerned about objective treatment of MESSA.
There can be no doubt that any attempt to curtail MESSA will be a call-to-arms for the MEA. The union relies on MESSA as a way of controlling loyalty to the union; MEA members believe that they cannot obtain generous insurance benefits through MESSA without the MEA's sponsorship of the program. The MEA cannot afford to lose this control mechanism. Both MESSA and the MEA have the necessary resources to fight any attempt at restraining the MESSA operation. The MEA can manipulate many public officials through campaign contributions and political pressure, and MESSA has enough financial reserves to pay for legal services, lobbying staff, and other programs necessary to combat its opposition. Moreover, MESSA can recuperate the costs of self-defense by increasing premium rates, inducing more illegitimate taxpayer support.
Where does this leave taxpayers and school districts who do not have a powerful political mechanism for defending their interests? The MEA's political influence and lobbying funds will give it the strength to wage a battle in defense of MESSA. The only way Michigan's citizens and school districts can win is by resisting the union's political tactics, by openly voicing their concerns, and by heaping their own pressure on state legislators. Of course, success would require that public servants act in the best interest of parents and other taxpayers and steadfastly resist the MEA opposition. Identifying the problems of MESSA is not difficult; standing up to the MEA is.
The problems posed by the MEA/MESSA relationship are testimony to the fact that the MEA dominates public education at both the state and school district level. The balance of power has clearly shifted to the point where school districts find themselves at a severe disadvantage in instituting sound labor agreements without a prolonged and disruptive strike. The following policies would create a more responsible environment for public school employment:
1. Exempt public school teachers from the Public Employment Relations Act (PERA).
Since 1966, school districts have been forced through the PERA to bargain insurance benefits and other terms and conditions of employment with the MEA's affiliates. School districts should be able to deal freely and directly with their employees without the state-sanctioned pressure of the MEA. Teachers should be allowed to join a union, but not be forced into membership or support. This would help restore a more equal and responsible relationship between school districts and their employees.
2. At the very least, amend PERA to exempt insurance and benefits as mandatory topics of bargaining.
If legislators are unable to exempt public school teachers completely, they should at least exempt insurance and benefits from mandatory collective bargaining. School districts would still be required to bargain wages and other conditions of employment, but they would have more freedom to select insurance providers based on cost and merit, not political pressure.
3. Require school districts to competitively bid insurance providers, and have those providers supply claims information.
Although this is less desirable than the first two recommendations, a state law that requires school - districts to competitively bid insurance providers would help prevent abuse of state-sanctioned mandatory collective bargaining. Such a law should include requirements that the provider or underwriter provide a complete claims history.
Michigan House of Representatives
James Agee (D-Muskegon)
Dick Allen (R-Caro)
Tom Alley (D-West Branch)
David Anthony (D-Escanaba)
Paul T. Baade (D-Muskegon)
Lyn Bankes (R-Redford)
Justine Barns (D-Westland)
Robert Bender (R-Middleville)
Michael J. Bennane (D-Detroit)
Maxine Berman (D-Southfield)
Bill Bobier (R-Hesperia)
Beverly Bodem (R-Alpena)
Robert Brackenridge (R-St. Joseph)
Mary C. Brown (D-Kalamazoo)
William R. Bryant, Jr. (R-Grosse Pointe Farms)
Willis C. Bullard, Jr. (R-Milford)
Dianne Byrum (D-Holt)
Nick Ciaramitaro (D-Roseville)
Floyd Clack (D-Flint)
Candace A. Curtis (D-Swartz Creek)
Robert A. DeMars (D-Lincoln Park)
Barbara J. Dobb (R-Commerce Twp.)
Agnes Dobronski (D-Dearborn)
Jan C. Dolan (R-Farmington Hills)
Robert L. Emerson (D-Flint)
Frank M. Fitzgerald (R-Grand Ledge)
Pat Gagliardi (D-Drummond Island)
John Gemaat (R-McBain)
Donald H. Gilmer (R-Augusta)
Sharon L. Gire (D-Clinton Township)
Carl F. Gnodtke (R-Sawyer)
Michael J. Griffin (D-Jackson)
David M. Gubow (D-Huntington Woods)
Clark Harder (D-Owosso)
Charlie J. Harrison, Jr. (D-Pontiac)
Curtis Hertel (D-Detroit)
Paul C. Hillegonds (R-Holland)
David C. Hollister (D-Lansing)
Morris W. Hood, Jr. (D-Detroit)
Dominic J. Jacobetti (D-Negaunee)
Shirley Johnson (R-Royal Oak)
H. Lynn Jondahl (D-Okemos)
William R. Keith (D-Garden City)
Carolyn C. Kilpatrick (D-Detroit)
Burton Leland (D-Detroit)
Terry London (R-Marysville)
Bill Martin (R-Battle Creek)
Thomas C. Mathieu (D-Grand Rapids)
Jim McBryde (R-Mt. Pleasant)
James McNutt (R-Midland)
James Mick Middaugh (R-Paw Paw)
Thomas Middleton (R-Ortonville)
Raymond M. Murphy (D-Detroit)
Michael E. Nye (R-Litchfield)
Dennis Olshove (D-Warren)
James E. O'Neill (D-Saginaw)
Lynn Owen (D-Monroe)
Glenn Oxender (R-Sturgis)
Joseph Palamara (D-Wyandotte)
Gregory E. Pitoniak (D-Taylor)
Vincent Joe Porreca (D-Trenton)
Kirk A. Profit (D-Ypsilanti)
Gary L. Randall (R-Elwell)
Lynn N. Rivers (D-Ann Arbor)
Sal Rocca (R-Sterling Heights)
Nelson W. Saunders (D-Detroit)
Mary Schroer (D-Ann Arbor)
Thomas E. Scott (D-Burton)
Steven Shepich (D-Iron River)
Dale L. Shugars (R-Portage)
Ken Sikkema (R-Grandville)
Alma G. Stallworth (D-Detroit)
Ted Wallace (D-Detroit)
Lloyd "Pete" Weeks (D-Warren)
Howard Wetters (D-Kawkawlin)
Tracey A.. Yokich (D-St. Clair Shores)
Joseph F. Young, Jr. (D-Detroit)
Richard A. Young (D-Dearborn Heights)
Michigan Senate
Jim Berryman (D-Adrian)
Michael J. Bouchard (R-Birmingham)
John D. Cheffy, Jr. (D-Clio)
Jon Cisky (R-Saginaw)
Joe Conroy (D-Flint)
Dan L. DeGrow (R-Port Huron)
Fred Dillingham (R-Fowlerville)
Mat Dunaskiss (R-Oxford)
Vernon J. Ehlers (R-Grand Rapids)
Jack Faxon (D-Farmington Hills)
R. Robert Geake (R-Northville)
George Z. Hart (D-Dearborn)
Donald W. Koivisto (D-Ironwood)
George A. McManus, Jr. (R-Traverse City)
Michael J. O'Brien (D-Detroit)
Dick Posthumus (R-Alto)
Debbie Stabenow (D-Lansing)
Paul Wartner (R-Portage)
Michigan Supreme Court
Conrad Mallet, Jr. (Detroit)
Source: Filings of the Michigan Education Association Political Action Committee with the Bureau of Elections within the Michigan Department of State, covering the time period between January l4, 1992 and December 22, 1992.
|
Airport Community Schools |
MESSA |
For the reader's interest, an actual example of one school district's experience with MESSA has been included. Of course, every situation where a school district encounters the MESSA issue is uniquely resolved. In some instances, school district officials will yield to the teachers' union without a battle, and even purchase MESSA coverage for themselves. Other times, the fight over MESSA can become so intense that the union will strike for protracted lengths of time or the district will steadfastly resist MESSA. The example of the Troy School District was chosen because it represents a fair and accurate portrayal of what a school district may experience when negotiating MESSA insurance with an MEA local affiliate. The following discussion relates to the Troy School District's collective bargaining agreement for the 1990-93 school years. The district is now in the process of negotiating a successor contract.
Background
Prior to its 1990 health insurance agreement, the Troy School District gave its teachers the option of either MESSA Super Care II, a less comprehensive Blue Cross plan, or a $900 annuity in place of health insurance. For the insurance options, the district paid the full premium for single person, two-person, and full-family coverage. Of the 650teachers in the district, 570 were enrolled in MESSA, 17 were enrolled in Blue Cross, and83 opted to receive the cash annuity. Of the 567 teachers who selected health insurance,107 chose single-person coverage, 113 chose two-person coverage, and 367 chose full-family coverage.
In 1989, MESSA and Blue Cross announced that school districts could no longer offer competing insurance plans to their employees. The plan administrator with 25 percent or less of the enrollees had to withdraw from that particular market. In the Troy case, Blue Cross withdrew.
Impact of Teacher Costs on the Troy School District
For the Troy School District, the total cost of employee compensation was accelerating at an upward rate. Part of this cost increase could be attributed to the rising cost of employee health insurance. For example, the monthly premium for full-family MESSA health insurance increased at an average rate of 23 percent per year during a 10-year period, from $151.12 in 1980 to $538.66 in 1986. After accounting for salaries and other benefits, the district was paying around $30 million in teacher compensation. The average cost alone of a teacher with full-family MESSA coverage was $57,454.88.
As a consequence of these high costs, the Troy School Board acknowledged that it could not maintain its current level of educational programs if expenses continued to rise. The district's bargaining representatives were instructed to contain costs in any subsequent contracts negotiated with the teachers' union, particularly in the area of employee health insurance.
| Average Salary | $47,198.00 |
| Retirement benefits (MPSERS) | $2,359.90 |
| Health insurance | $6,463.92 |
| Dental insurance | $739.32 |
| Vision insurance | $196.68 |
| LTD insurance | $401.18 |
| Life insurance | $95.88 |
| Total average cost | $57,454.88 |
The Collective Bargaining Process with the Union
On May 1, 1990, the Troy Board of Education and the Troy Education Association began to negotiate a new labor contract. The contract talks concluded on May 24, 1991. During this389-day period, there were over 55 bargaining sessions, a 14-day teacher strike, two mediators from the Michigan Employment Relations Commission, and one court-appointed mediator. The foremost cause of the disputes was union resistance to the district's cost-containment suggestions. In order to maintain its educational programs and minimize costs, the district considered many strategies for cost-containment in the area of employee health insurance, including:
Reduce the total amount of employee benefits.
Limit the district's contributions toward health insurance premiums.
Require employees to pay a portion of the premium cost.
Restrict coverage to employees and have them pay for additional family members.
Provide managed care options, such as a health maintenance organization or a preferred provider organization.
Provide a "cafeteria plan," whereby teachers select coverage from various health benefits and cash alternatives.
Switch to comparable coverage from another provider.
Self-fund an insurance program.
The union opposed all of these measures and would not accept anything other than MESSA coverage. After considering the circumstances, the district chose to maintain the level of benefits already provided to teachers with MESSA insurance while seeking out the most efficient way to deliver the benefits.
If the district had purchased MESSA Super Care II for all teachers, the monthly premium rates per participant and annual costs for all participants would have been as follows:
| Monthly Premium Per Participant | Total Annual Cost For All Participants | |
|---|---|---|
| Single-person coverage | $211.15 | $271,117 |
| Two-person coverage | $495.42 | $671,790 |
| Full-family coverage | $538.66 | $2,372,259 |
With 107 single-person participants, 113 two-person participants, and 367 full-family participants, the total annual cost to the District would have been $3,315,166.
The district also considered purchasing the slightly less expensive Super Care I plan from MESSA. The only difference in coverage between the plans was that Super Care I required an annual deductible of $50 for individuals and $100 for families along with a$2.00 co-payment per prescription. The difference in premiums, on the other hand, was drastic:
| Super Care I | Super Care II | Difference | |
|---|---|---|---|
| Single-person coverage | $197.58 | $211.15 | $13.57 |
| Two-person coverage | $442.08 | $495.42 | $53.34 |
| Full-family coverage | $491.03 | $538.66 | $47.63 |
On an annual basis, the district would have saved a total of $299,515.44 by purchasing Super Care I instead of Super Care II. The average additional cost per teacher with the Super Care II plan would have been $510.25. Yet, MESSA only charged nominal deductibles and co-payments with Super Care 1, which otherwise offered the same coverage as Super Care II. The district could have made up the slight difference in coverage by reimbursing each teacher for the annual deductible and by providing a fund to cover the cost of prescriptions. If the district gave each teacher $125 to cover deductibles and prescriptions, the teachers would receive the exact same benefits as Super Care II and the district would save $226,140.44.
As part of its search for an efficient insurance provider, the district asked Group Benefit Services, Inc., its third-party administrator of insurance for support personnel, to submit a "self-funding" proposal that would cover all district employees. The coverage would have been identical to MESSA Super Care II, but would have cost only$2,596,200:
| Monthly Premium Per Participant | Total Annual Cost For All Participants | |
|---|---|---|
| Single-person coverage | $250.00 | $321,000 |
| Two-person coverage | $395.00 | $535,620 |
| Full-family coverage | $395.00 | $1,739,580 |
After adding in $7,748 to provide for equivalent life insurance coverage to what MESSA was offering with the Super Care II plan, the total cost to the district would have been$2,603,948-a savings of $711,218 over the MESSA plan. As a safety option if the union rejected the self-funding proposal, the district offered to provide MESSA coverage on the condition that MESSA supply evidence of the number of claims filed by the district's teachers so the School Board could assess the value of MESSA coverage. The teachers' union rejected both proposals.
The Troy Education Association would only settle on MESSA Super Care II or MESSA PAK coverage with Super Care I health insurance. The MESSA PAK option combines health, life, disability, vision, and dental insurance into optional packages, making MESSA the administrator of other coverages in addition to health coverage. In short, MESSA PAK aims to provide one complete employee insurance package rather than separate purchases of separate plans. Although the union claimed that MESSA PAK would save the district two percent of its total insurance costs, MESSA would not provide the verifying cost breakdown.
Of the two MESSA PAK plans offered to the district, Plan A was for teachers who required health coverage and Plan B was for teachers who did not need it. MESSA only offered composite rates for each plan, rather than rates based upon single-person, two-person, or full-family coverage. With 587 participants for Plan A and 90 participants for Plan B, the cost of MESSA PAK was as, follows:
| Monthly Premium | Total Annual Cost | |
|---|---|---|
| MESSA PAK Plan A | $558.88 | $3,936,751 |
| MESSA PAK Plan B | $145.80 | $157,464 |
After adding in $9,000 for a separately purchased annuity for teachers who did not require health insurance and deducting $1,095,328 for separately provided insurance, the total cost of the MESSA PAK program was $3,007,887-a savings of $307,279 over MESSA Super Care II.
In the end, the Troy Education Association and the Troy Board of Education agreed to MESSA PAK with MESSA Super Care I as the health coverage. The District offered to pay $125to each teacher who requested health coverage as reimbursement for prescriptions and deductibles. The district also reserved the right to terminate MESSA PAK if it could prove that the same life and disability coverage was available elsewhere at a lower cost.
1 Peter Brimelow and Leslie Spencer, "The National Extortion Association?" Forbes, June 7, 1993, p. 74.
2 Section 2 of the Public Employment Relations Act (MCL 423.202) states "No person holding a position by appointment or employment… in the public school service... shall strike."
3 For reference, see the notes to MESSA's financial statements regarding related party transactions.
4 The MEA also operates the Michigan Education Association Legal Services (MEALS) program. MEALS was formed through a fund established by the MEA, the NEA, and the State Bar of Michigan, and began operating in 1974. The program was created as a negotiated fringe benefit in labor contracts which would provide pre-paid legal services to teachers.
5 Michigan Association of School Boards, "Questions and Answers About Health Insurance Bidding in Michigan's Public Schools," May 14, 1991, p. 2.
6 Michigan Association of School Boards, "Questions and Answers About Health Insurance Bidding in Michigan's Public Schools," May 14, 1991, p. 2.
7 Society of Professional Benefit Administrators, Directory of Third Party Administration Firms, 1993, p. 114.
8 For reference, see Section 501(c)(9) of the Internal Revenue Code.
9 Stated in the "Decision and Recommended Order of Administrative Law Judge" in the case of St. Clair Intermediate School District v. IEA/MEA and MESSA, MERC Case No. CU90 H-33,1992, p.3.
10 Peter Brimelow and Leslie Spencer, "The National Extortion Association?" Forbes, June 7, 1993, p. 81.
11 MESSA document, "MESSA Layoff Benefit Plan," dated July 12, 1982.
12 Brief of Appellant Michigan Education Special Services Association, IEA/MEA and MESSA v. St. Clair Intermediate School District, Michigan Court of Appeals Docket Nos. 161643 and 161645, p. 8.
13 The case of the Brandon School District, et al., v. Michigan Education Association, et al. (Insurance Bureau File No. 88-9510-L, September 6, 1985), was predominantly defended on the grounds that the Insurance Code does not apply to MESSA.
14 Houghton Lake Education Association v. Houghton Lake Board of Education, 109 Mich App 1 (1981)
15 MEA/NEA v. St. Charles Community Schools, 150 Mich App 763 (1986).
16 IEA/MEA and MESSA v. St. Clair Intermediate School District, Michigan Court of Appeals Docket Nos. 161643 and 161645.
17 For reference, see the "Governance Documents" of the Michigan Education Association (File No. 512840), last revised in May of 1991, available from the Office of Labor Management Standards within the U.S. Department of Labor.
18 Survey of MEA members, "MEA Evaluation," Greenberg-Lake: The Analysis Group, Inc., Washington D.C., March 1989, p.2.
19 Based upon information provided in the "Summary of Benefits" forms for various MESSA plans, distributed by the Michigan Education Association, dated April of 1990.
20 Houghton Lake Education Association v. Houghton Lake Board of Education, 109 Mich App 1 (1981).
21 MEA document: "MESSA and the MEA member in partnership together," dated April of 1989.
22 Peter Brimelow and Leslie Spencer, "The National Extortion Association?" Forbes, June 7, 1993, p. 82.
23 MEA document: "Labor Organization Annual Report, Form LM-2," filed with the U.S. Department of Labor, Office of Labor Management Standards, dated November 26, 1992, Item 38.
24 Houghton Lake Education Association v. Houghton Lake Board of Education, 109 Mich App 1 (1981).
25 Michigan Association of School Boards, "Helping Reduce Health Insurance Costs," MASB Summer Academies, 1991.
26 Memorandum from Reg Rye, Superintendent of Hemlock Public Schools, to Larry Engel, Superintendent of the Saginaw Intermediate School District, dated February 12, 1993.
27 For reference, see Brandon School District, et al. v. Insurance Commissioner, et al., Michigan Court of Appeals Docket No. 126891
28 MESSA document, "Notice: Information Concerning MESSA Health Plans," dated April 9, 1985, p. 7.
29 Calculated as follows: Five percent savings from elimination of Equitable rate increases plus seven percent savings from conversion to BCBSM.
30 Post-Hearing Brief of Charging Party St. Clair Intermediate School District, St. Clair Intermediate School District v. IEA/MEA and MESSA, Michigan Employment Relations Commission Administrative Law Court, MERC Case No. CU90 H-33, p. 13-14.
31 Petition for a Contested Case, Brandon School District, et al., v. Michigan Education Association, et al., Insurance Bureau File No. 88-9510-L, September 6, 1985, p. 12.
32 Beverly Wolkow, "Report on 1985-86 - Year of Many MEA Accomplishments for Members," The Voice, May 26, 1986, p. 2.
33 MESSA document, "Marketing and Service Program Agreement," dated August 3, 198 1, p. 2.
34 Michigan Association of School Boards, "Helping to Reduce the Cost of Health Insurance," MASB Legislative Relations Network, 1992, p. 16.
35 Michigan Chamber of Commerce, Property Taxes & School Finance: What Happens Next?, "Cost Containment," July 30, 1993, p. 8.
36 Michigan Association of School Boards, "Helping Reduce Health Insurance Costs," MASB Summer Academies, 1991.
37 Hospital Council of East Central Michigan, "Facts That Direct Policy," March 8, 1991, p. 5.
38 Michigan Association of School Boards, "Health Care Costs," MASB Legislative Relations Network, 1991, p. 20.
39 Excerpted from "Summary of Benefits" forms for various MESSA plans, distributed by the Michigan Education Association, dated April of 1990.
40 Peter Brimelow and Leslie Spencer, "The National Extortion Association?" Forbes, June 7, 1993, p. 82.
41 Richard Cantley, "A Report and Commentary on the Michigan Education Special Services Association: Prepared by a Michigan Taxpayer," 1991, p. 3.
42 Peter Brimelow and Leslie Spencer, "The National Extortion Association?" Forbes, June 7, 1993, p. 82.
43 Editorial, "The MEA's Sweetheart Deals," The Detroit News, March 7, 1993, p. 2B.
44 Mike Thompson, "Insurance Switch Keys Teacher Pact," The Saginaw News, June 2, 1993, p. Al.
45 Letter from the Michigan Association of School Boards to Attorney General Frank Kelley, dated October 6, 1989, p. 3.
46 Michigan Association of School Boards, "Helping Reduce the Cost of Health Insurance," MASB Legislative Relations Network, 1992, p. 17.
47 Letter from Deputy Comn-tissioner Jean K. Carlson of the Insurance Bureau to Robert Kasperek of BCB SM, dated December 15, 1992.
48 MESSA document, "Notice: Information Concerning MESSA Health Plans," dated April 9, 1985, p. 1-2.
49 Letter from the law firm of Fraser, Trebilock, Davis & Foster, P.C., to Comn-tissioner Herman W. Coleman, dated October 4, 1985.
50 Based upon information listed in "Michigan Education Special Services Association: Schedule of Operating Expenses," located as the last section of MESSA financial statements.
51 Peter Brimelow and Leslie Spencer, "The National Extortion Association?" Forbes, June 7, 1993, p. 82.
52 MESSA document, "Notice: Information Concerning MESSA Health Plans," dated April 9, 1985, p. 5.
53 Public Sector Consultants, "Health Care Costs and Mandated Benefits," Michigan Insurance Handbook, 1993, p. 107.
54 MESSA document, "Notice: Information Concerning MESSA Health Plans," dated April 9,1985. p. 7.
55 Public Sector Consultants, Michigan Insurance Issues Handbook, Public Sector Consultants, Inc., 1993, p. 111.
56 Blue Ribbon Committee on Health Care and Business, "Exploring Areas of Mutual Interest and Benefit," Hospital Council of East Central Michigan, March 8, 1991, p. 13.
51 Peter Brimelow and Leslie Spencer, "The National Extortion Association?" Forbes, June 7, 1993, p. 82.
58 MESSA document, "Background Summary," accompanied Insurance Bureau filing dated December 4, 1985, p. 1.
59 Letter from Fraser Trebilock Davis & Foster P.C. to Insurance Commissioner Herman W. Coleman, October 4, 1985. This letter discusses the Formula II document on file with the Michigan Insurance Bureau, which can also be obtained as a public document.
60 MASB Legislative Relations Network, "Health Care Costs," 1991, p. 20
61 For reference, see Section 8 of the federal Clayton Antitrust Act of 1914.
62 For reference, see the federal McCarran-Ferguson Act of 1945 and Michigan's Antitrust Reform Act (Public Act 274 of 1984).
63 Letter from Steven Hess of the BCBSM Office of the General Counsel to Wallace Long of Cox & Hodgman, P.C., dated September 4, 1992.
64 Letter from Wallace Long of Cox & Hodgman, P.C., to Commissioner David Dykhouse of the Michigan Insurance Bureau, dated July 6, 1992.
65 Letter from Keith Provost, Assistant Superintendent of Clawson School District to Senator Jack Welborn, dated May 22, 1991.
66 Letter from Iris Socolofsky of Fraser, Trebilock, Davis,. & Foster P.C. to Attorney General Frank Kelley, dated December 1, 1989.
67 Letter from Bridget E. Hughes of the Jardine Insurance Agency to Mara Jane Zodtner of the Troy School District, dated September 4, 1990.
68 MESSA document, "Employer Participation Agreement for Negotiated Group Benefit Programs," dated 1989.
69 MESSA document, "Employer Participation Agreement for Negotiated Group Benefit Programs," dated 1989.
70 MESSA document, "Employer Participation Agreement for Negotiated Group Benefit Programs," dated 1989.
71 Stated in "Decision and Order of Appeals Commission," in the case of St. Clair Intermediate School District v. IEA/MEA and MESSA, MERC Case No. CU90 H-33, p. 3.
72 The legal basis of this case pertained to a violation of Section 10(3)(c) of the Public Employment Relations Act, MCL 423.201 et seq.
73 Stated in the "Decision and Recommended Order of Administrative Law Judge" in the case of St. Clair Intermediate School District v. IEA/MEA and MESSA, MERC Case No. CU90 H-3 3, 1992, p. I 1.
74 Stated in "Decision and Order of Appeals Commission," in the case of St. Clair Intermediate School District v. IEA/MEA and MESSA, MERC Case No. CU90 H-33, p. 5.
75 Michigan Association of School Boards, "Questions and Answers About Health Insurance Bidding in Michigan's Public Schools," May 14, 199 1, p. 2.
76 Maureen Kelly and John Gierak, "Summary of Health Insurance Issue for the 1990-93 Troy Teachers Contract," Mosher, Vondale, Gierak, & Baumhart, P.C., July 9, 199 1, p. 9. National Education Association, "State Side: Midwest," NEA Today, April 1983, p. 7.
77 National Education Association, "State Side: Midwest," NEA Today, April1983, p. 7.
78 MESSA document, "Report on Financial Statements: Years Ended November 30, 1984 and 1983," p. 9.
79 Letter from the Michigan Association of School Boards to Attorney General Frank Kelley, dated October 6, 1989. ,
80 Letter from Richard Whitmer, President of BCBSM, to Stephen Wang, Assistant Superintendent of Mt. Morris Consolidated Schools, dated September 25, 1989.
81 Editorial, "The MEA's Sweetheart Deals," The Detroit News, March 7, 1993, p. 2B.
82 Copperweld Corporation v. Independence Tube Corporation, 467 U.S. 752 (1984)
83 MESSA document, "Articles of Incorporation," Section 11, as of September 9, 1960.
84 MESSA document, "Bylaws of Michigan Education Special Services Association," Article 1, Section 1, as of October II, 1985.
85 MEA document, "MESSA and the MEA member in partnership together," dated April, 1989.
86 Stated in the "Decision and Recommended Order of Administrative Law Judge" in the case of St. Clair Intermediate School District v. IEA/MEA and MESSA, MERC Case No. CU90 H-33,1992, p. 3.
87 MESSA document, "Bylaws of Michigan Education Special Services Association,". Article IV, Section 8, as of October 11, 1985. A quorum at all meetings of trustees is defined therein as "a majority of incumbent trustees." No motion may be passed without this quorum.
88 MESSA document, "Bylaws of Michigan Education Special Services Association," Article 11, Section 7, as of October 11, 1985.
89 MESSA document, "Bylaws of Michigan Education Special Services Association',". Article III, Section 3, as of October 11, 1985.
90 Sworn testimony of Beverly Wolkow; Post-Hearing Brief of Charging Party St. Clair Intermediate School District, St. Clair Intermediate School District v. IEA/MEA and MESSA, Michigan Employment Relations Commission Administrative Law Court, MERC Case No. CU90 H-33, p. 10.
91 Brief of Appellant Michigan Education Special Services Association, IEA/MEA and MESSA v. St. Clair Intermediate School District, Michigan Court of Appeals Docket Nos. 161643 and 161645, p. 8.
92 Stated in the "Decision and Recommended Order of Administrative Law Judge" in the case of St. Clair Intermediate School District v. IEA/MEA and MESSA, MERC Case No. CU90 H-33,1992, p. 9.
93 Post-Hearing Brief of Charging Party St. Clair Intermediate School District, St. Clair Intermediate School District v. IEA/MEA and MESSA, Michigan Employment Relations Commission Administrative Law Court, MERC Case No. CU90 H-33, p. 13.
94 MEA document, "Annual Report 76-77," dated 1977, p. 28.
95 Petition for a Contested Case, Brandon School District, et al., v. Michigan Education Association, et al., Insurance Bureau File No. 88-9510-L, September 6, 1985, p. 31. 96
96 Maureen Kelly and John Gierak, "Summary of Health Insurance Issue for the 1990-93 Troy Teachers Contract," Mosher, Vondale, Gierak, & Baumhart, P.C., July 9, 1991, p. 10.
97 Senator Jack Welborn, "The Fury of a Vested Interest," Right to the Point, May 9, 1991.
98 Letter from Iris Socolofsky of Fraser, Trebilock, Davis & Foster, P.C., to Attorney General Frank Kelley, dated December 1, 1989.
99 MEA document, "MESSA and the MEA member in partnership together," dated April, 1989.
100 MCL 423.202 (Section 2 of the Public Employment Relations Act) states "No person holding a position by appointment or employment...in the public school service... shall strike."
101 Stated in the "Decision and Recommended Order of Administrative Law Judge" in the case of St. Clair Intermediate School District v. IEA/MEA and MESSA, MERC Case No. CU90 H-33,1992, p. 10.
102 For reference, see Fraternal Order of Police v. Meridian Township, 90 Mich App 533 (1979); and Stephenson v. Golden, 279 Mich 710 (1937).
103 Brief of Appellant Michigan Education Special Services Association, IEA/MEA and MESSA v. St. Clair Intermediate School District, Michigan Court of Appeals Docket Nos. 161643 and 161645, p. 21.
104 Calculated as follows: Payments to MEA + Payments to MEDNA Revenues in excess of benefit costs [($1,549,000 + $28,500 + $8,285,000) -, $27,865,559] 35.4 percent
105 For reference, see the "Michigan Annual Report - Profit Corporations," filed by the Michigan Education Data Network Association with the Michigan Department of Commerce.
106 Information contained herein was taken from the "MEA/MESSA Marketing and Service Program Agreement," dated August 3, 1981.
107 MESSA document, "MEA/MESSA Marketing and Service Program Agreement," dated August 3, 198 1, p. 1.
108 Brief of Appellant Michigan Education Special Services Association, IEA/MEA and MESSA v. St. Clair Intermediate School District, Michigan Court of Appeals Docket Nos. 161643 and 161645, p. 9.
109 MESSA document, "MEA/MESSA Marketing and Service Program Agreement," dated August 3, 1981, p. 2.
110 MESSA document, "Addendum to the MEA/MESSA Marketing and Service Program Agreement," dated August 3, 1981.
111 MESSA document, "MESSA and the MEA Member in Partnership Together," dated April of 1989, p. 2.
112 MESSA document, "Addendum to the MEA/MESSA Marketing and Service Program Agreement," dated August 3, 1981.
113 MESSA document, "MEA/MESSA Marketing and Service Program Agreement," dated August 3, 1981, p. 2.
114 The MEA also receives a substantial cash flow from MESSA's annual rental payments. According to MESSA's financial statements, MESSA has been leasing a parcel of land from the MEA since April 1, 1975. The lease will expire on March 31, 2074. The annual base rate is $20,000, not including adjustments for inflation.
115 MEDNA document, "Articles of Incorporation," Article II, dated November 24, 1982.
116 Brief of Appellant Michigan Education Special Services Association, IEA/MEA and MESSA v. St. Clair Intermediate School District, Michigan Court of Appeals Docket Nos. 161643 and 161645, p. 9.
117 Based upon the figures for MEDNA's total income identified in the MEA's "Return of Organization Exempt From Income Tax: IRS Form 990," and MESSA's total payment to MEDNA for services identified in MESSA financial statements.
118 Mark Hornbeck, "State reviews teachers' insurance costs," The Detroit News, September 22, 1993, p. B 1.
119 Michigan Association of School Boards, "Memo to members of the MASB Legislative Relations Network," dated May 14, 199 1.
120 Determined from MEA PAC filings with the Bureau of Elections for the period covering January 14, 1991 to December 22, 1992
121 Governor Engler addressed the monopoly on health insurance for the school employees of Michigan in "A Prescription for a Healthy Michigan: Special Message on Health Care," dated March 11, 1992. Senator Jack Welborn has commented on MESSA in his "Right to the Point" column and in letters to his constituents. '
122 Despite numerous requests that his office investigate MESSA, Attorney General Kelley has avoided the issue. For example, Senator Welborn sent a request dated to January 27, 1990, to the Attorney General asking for an investigation of MESSA. Over a year had lapsed without a reply, and the Senator repeated his request to the Attorney General. An aide for Senator Welborn confirmed in June of 1993 that the investigation was expected to begin as soon as the Attorney General's office found the time.
123 Excerpted from a profile of NEA President Keith Geiger, printed by Concerned Educators Against Forced Unionism
124 MEA filing, "Statement of Organization, Campaign Finance Reporting," dated June 28, 1977, Section 7.
125 Excerpted from a profile of NEA President Keith Geiger, printed by Concerned Educators Against Forced Unionism
126 Letter from' Kevin S. Harty of Tbrun, Maatsch, and Nordberg, P.C. to Commissioner Herman Coleman, dated October 4, 1992.
127 Letter from Commissioner Herman Coleman to Kevin S. Harty of Tbmn, Maatsch, and Nordberg, P.C., dated October 9, 1985.
128 Letter from Thrun, Maatsch, and Nordberg, P.C. to Attorney General Frank Kelley, dated October 6, 1989.